Journal Description
Dermatopathology
Dermatopathology
is an international, peer-reviewed, open access journal on dermatopathology. The journal is owned by the European Society of Dermatopathology (ESDP) and is published quarterly online by MDPI (since Volume 7 Issue 1 - 2020).
- Open Access— free for readers, with article processing charges (APC) paid by authors or their institutions.
- High visibility: indexed within ESCI (Web of Science), PubMed, PMC, Embase, and other databases.
- Rapid Publication: manuscripts are peer-reviewed and a first decision is provided to authors approximately 29.9 days after submission; acceptance to publication is undertaken in 3.9 days (median values for papers published in this journal in the second half of 2023).
- Recognition of Reviewers: APC discount vouchers, optional signed peer review, and reviewer names published annually in the journal.
Impact Factor:
1.9 (2022);
5-Year Impact Factor:
1.3 (2022)
Latest Articles
Poikilodermatous Plaque-like Hemangioma: Case Presentation and Literature Review
Dermatopathology 2024, 11(2), 147-153; https://doi.org/10.3390/dermatopathology11020015 - 21 May 2024
Abstract
Poikilodermatous plaque-like hemangioma (PPH) is a recently described clinical and pathological entity, with only 18 cases reported in the literature. Although uncommon, this benign condition presents consistent clinical and histological findings. We present a new case of PPH in an 81-year-old male and
[...] Read more.
Poikilodermatous plaque-like hemangioma (PPH) is a recently described clinical and pathological entity, with only 18 cases reported in the literature. Although uncommon, this benign condition presents consistent clinical and histological findings. We present a new case of PPH in an 81-year-old male and review the existing literature. The persistence over time and the need to distinguish PPH from more significant lesions underscore the importance of its clinical and pathological recognition.
Full article
(This article belongs to the Section Clinico-Pathological Correlation in Dermatopathology)
►
Show Figures
Open AccessCase Report
Intratarsal Keratinous Cyst Clinically Misdiagnosed as a Chalazion
by
John Lennon Silva Cunha, Clenia E. S. Andrade, Fernando A. P. da Cunha Filho, Alexandre R. da Paz, Manuel A. Gordón-Núñez, Pollianna M. Alves and Cassiano F. W. Nonaka
Dermatopathology 2024, 11(2), 142-146; https://doi.org/10.3390/dermatopathology11020014 - 19 Apr 2024
Abstract
The intratarsal keratinous cyst (IKC) is a recently described entity, often clinically misdiagnosed as a chalazion. We report a case of a 61-year-old male patient with a chief complaint of a small lesion on the upper eyelid that evolved over six months. On
[...] Read more.
The intratarsal keratinous cyst (IKC) is a recently described entity, often clinically misdiagnosed as a chalazion. We report a case of a 61-year-old male patient with a chief complaint of a small lesion on the upper eyelid that evolved over six months. On physical examination, an asymptomatic, firm nodule was identified on the left upper eyelid. The patient reported no history of trauma. A provisional diagnosis of chalazion was established, and an excisional biopsy was performed. Histopathologically, the lesion was lined with a stratified squamous epithelium, with a corrugated epithelial surface showing abrupt keratinization without keratohyalin granules, and compact keratinous-appearing material in the cystic lumen. The diagnosis was IKC. No signs of recurrence were observed after one year of follow-up. It is essential to accurately diagnose IKC and distinguish it from chalazion and epidermal inclusion cysts, because IKC requires complete surgical excision and can exhibit multiple recurrences if not properly removed.
Full article
(This article belongs to the Special Issue Educational Case Reports in Dermatopathology)
►▼
Show Figures
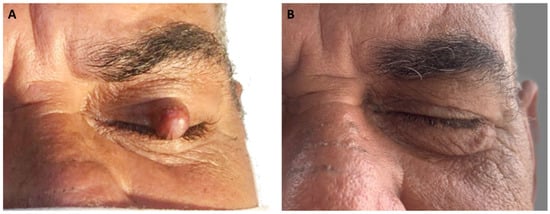
Figure 1
Open AccessArticle
Cutaneous Reactions after COVID-19 Vaccines: Analysis of the Clinical and Histopathological Spectrum—Case Series and Review of the Literature
by
Ursina Schmid, Jörg Galambos, Katrin Pfaltz, Ivan Hegyi, Salomé Courvoisier and Werner Kempf
Dermatopathology 2024, 11(1), 130-141; https://doi.org/10.3390/dermatopathology11010013 - 14 Mar 2024
Abstract
(1) Background: Various cutaneous adverse drug reactions (ADRs) are observed with the implementation of mRNA COVID-19 vaccines. To gain insight into the clinicopathologic features, we analyzed the correlation of histological and clinical data in 48 patients with these ADRs. (2) Methods: Single-center retrospective
[...] Read more.
(1) Background: Various cutaneous adverse drug reactions (ADRs) are observed with the implementation of mRNA COVID-19 vaccines. To gain insight into the clinicopathologic features, we analyzed the correlation of histological and clinical data in 48 patients with these ADRs. (2) Methods: Single-center retrospective study in patients with ADRs after mRNA COVID-19 vaccination (mRNA-1273 and BNT162b2 vaccines). (3) Results: Distant generalized ADRs prevailed (91%), often appearing clinically as spongiotic dermatitis or maculopapular exanthema. Histopathological analysis revealed spongiotic changes (46%) and dermal superficial perivascular predominantly lymphocytic infiltrates (17%). Eosinophils were found in 66% of biopsies, neutrophils in 29%, and plasma cells only in 8% of biopsies. Most ADRs occurred after the second vaccine dose (44%). Histologically spongiotic changes were associated with clinical features of spongiotic dermatitis in only 50% of patients and maculopapular exanthema in the remaining patients. ADRs represented an aggravation of preexisting skin disease in 23% of patients. ADRs regressed within 28 days or less in 53% of patients and persisted beyond a month in the remaining patients. (4) Conclusions: Our study demonstrates a diverse spectrum of generalized ADRs, revealing correlations between histology and clinical features but also instances of divergence. Interestingly, in about half of our patients, ADRs were self-limited, whereas ADRs extended beyond a month in the other half.
Full article
(This article belongs to the Section Clinico-Pathological Correlation in Dermatopathology)
►▼
Show Figures
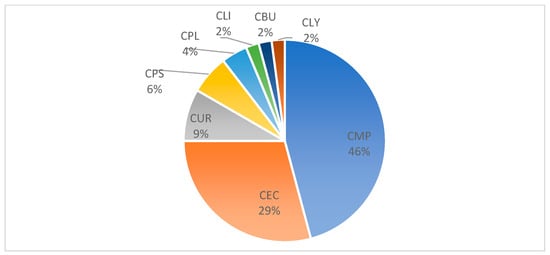
Figure 1
Open AccessEditorial
The Leading Impact Journal in Dermatopathology
by
Gürkan Kaya
Dermatopathology 2024, 11(1), 129; https://doi.org/10.3390/dermatopathology11010012 - 6 Mar 2024
Abstract
As the Editor-in-Chief of Dermatopathology and the President of the European Society of Dermatopathology (ESDP), I have the great pleasure of celebrating the 10th anniversary of Dermatopathology, the only online journal in the field of cutaneous pathology and the official journal of
[...] Read more.
As the Editor-in-Chief of Dermatopathology and the President of the European Society of Dermatopathology (ESDP), I have the great pleasure of celebrating the 10th anniversary of Dermatopathology, the only online journal in the field of cutaneous pathology and the official journal of the ESDP [...]
Full article
Open AccessCase Report
Sebaceomas in a Muir–Torre-like Phenotype in a Patient with MUTYH-Associated Polyposis
by
Julia Guarrera, James C. Prezzano and Kathleen A. Mannava
Dermatopathology 2024, 11(1), 124-128; https://doi.org/10.3390/dermatopathology11010011 - 4 Mar 2024
Abstract
►▼
Show Figures
This case report describes a case of a patient with MUTYH-associated polyposis (MAP), who presented with multiple sebaceomas in a Muir–Torre-like phenotype. MAP is caused by mutations in MUTYH, a base excision repair gene responsible for detecting and repairing the 8-oxo-G:A transversion caused
[...] Read more.
This case report describes a case of a patient with MUTYH-associated polyposis (MAP), who presented with multiple sebaceomas in a Muir–Torre-like phenotype. MAP is caused by mutations in MUTYH, a base excision repair gene responsible for detecting and repairing the 8-oxo-G:A transversion caused by reactive oxygen species. MAP is associated with an increased risk of developing adenomatous polyps and colorectal cancer. Muir–Torre syndrome is a clinical phenotype of Lynch syndrome, which presents with multiple cutaneous sebaceous neoplasms. Lynch syndrome, like MAP, increases the likelihood of developing colorectal cancer but with a different pathogenesis and mode of inheritance. This case demonstrates that in a patient presenting with multiple sebaceous neoplasms, further workup and genetic testing may be indicated, not only for Muir–Torre and Lynch syndrome but also for MAP.
Full article
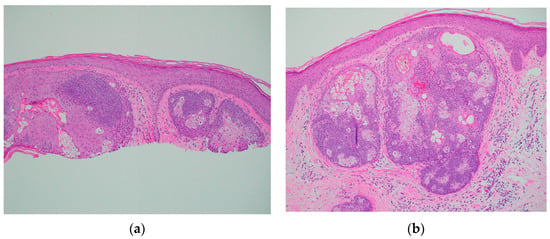
Figure 1
Open AccessReview
Kinase Fusions in Spitz Melanocytic Tumors: The Past, the Present, and the Future
by
Maged Daruish, Francesca Ambrogio, Anna Colagrande, Andrea Marzullo, Rita Alaggio, Irma Trilli, Giuseppe Ingravallo and Gerardo Cazzato
Dermatopathology 2024, 11(1), 112-123; https://doi.org/10.3390/dermatopathology11010010 - 14 Feb 2024
Abstract
►▼
Show Figures
In recent years, particular interest has developed in molecular biology applied to the field of dermatopathology, with a focus on nevi of the Spitz spectrum. From 2014 onwards, an increasing number of papers have been published to classify, stratify, and correctly frame molecular
[...] Read more.
In recent years, particular interest has developed in molecular biology applied to the field of dermatopathology, with a focus on nevi of the Spitz spectrum. From 2014 onwards, an increasing number of papers have been published to classify, stratify, and correctly frame molecular alterations, including kinase fusions. In this paper, we try to synthesize the knowledge gained in this area so far. In December 2023, we searched Medline and Scopus for case reports and case series, narrative and systematic reviews, meta-analyses, observational studies—either longitudinal or historical, case series, and case reports published in English in the last 15 years using the keywords spitzoid neoplasms, kinase fusions, ALK, ROS1, NTRK (1-2-3), MET, RET, MAP3K8, and RAF1. ALK-rearranged Spitz tumors and ROS-1-rearranged tumors are among the most studied and characterized entities in the literature, in an attempt (although not always successful) to correlate histopathological features with the probable molecular driver alteration. NTRK-, RET-, and MET-rearranged Spitz tumors present another studied and characterized entity, with several rearrangements described but as of yet incomplete information about their prognostic significance. Furthermore, although rarer, rearrangements of serine–threonine kinases such as BRAF, RAF1, and MAP3K8 have also been described, but more cases with more detailed information about possible histopathological alterations, mechanisms of etiopathogenesis, and also prognosis are needed. The knowledge of molecular drivers is of great interest in the field of melanocytic diagnostics, and it is important to consider that in addition to immunohistochemistry, molecular techniques such as FISH, PCR, and/or NGS are essential to confirm and classify the different patterns of mutation. Future studies with large case series and molecular sequencing techniques are needed to allow for a more complete and comprehensive understanding of the role of fusion kinases in the spitzoid tumor family.
Full article
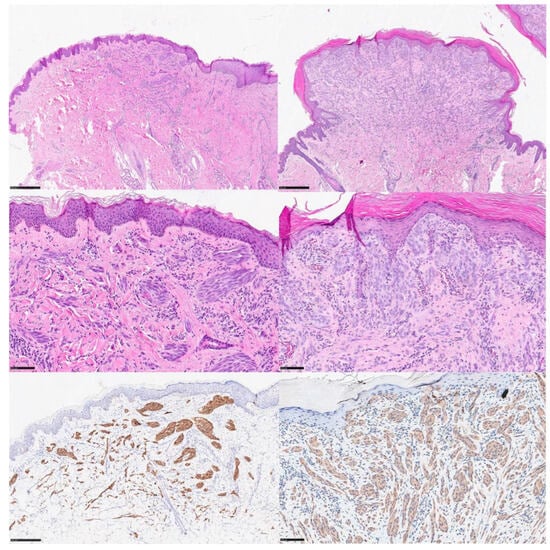
Figure 1
Open AccessReview
Skin and Syntax: Large Language Models in Dermatopathology
by
Asghar Shah, Samer Wahood, Dorra Guermazi, Candice E. Brem and Elie Saliba
Dermatopathology 2024, 11(1), 101-111; https://doi.org/10.3390/dermatopathology11010009 - 14 Feb 2024
Cited by 1
Abstract
This literature review introduces the integration of Large Language Models (LLMs) in the field of dermatopathology, outlining their potential benefits, challenges, and prospects. It discusses the changing landscape of dermatopathology with the emergence of LLMs. The potential advantages of LLMs include a streamlined
[...] Read more.
This literature review introduces the integration of Large Language Models (LLMs) in the field of dermatopathology, outlining their potential benefits, challenges, and prospects. It discusses the changing landscape of dermatopathology with the emergence of LLMs. The potential advantages of LLMs include a streamlined generation of pathology reports, the ability to learn and provide up-to-date information, and simplified patient education. Existing instances of LLMs encompass diagnostic support, research acceleration, and trainee education. Challenges involve biases, data privacy and quality, and establishing a balance between AI and dermatopathological expertise. Prospects include the integration of LLMs with other AI technologies to improve diagnostics and the improvement of multimodal LLMs that can handle both text and image input. Our implementation guidelines highlight the importance of model transparency and interpretability, data quality, and continuous oversight. The transformative potential of LLMs in dermatopathology is underscored, with an emphasis on a dynamic collaboration between artificial intelligence (AI) experts (technical specialists) and dermatopathologists (clinicians) for improved patient outcomes.
Full article
(This article belongs to the Special Issue Artificial Intelligence in Dermatopathology)
►▼
Show Figures
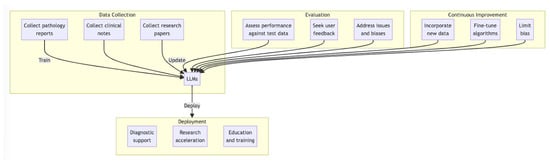
Figure 1
Open AccessReview
Galli–Galli Disease: A Comprehensive Literature Review
by
Andrea Michelerio, Antonio Greco, Dario Tomasini and Carlo Tomasini
Dermatopathology 2024, 11(1), 79-100; https://doi.org/10.3390/dermatopathology11010008 - 7 Feb 2024
Abstract
Galli–Galli disease (GGD) is a rare genodermatosis that exhibits autosomal dominant inheritance with variable penetrance. GGD typically manifests with erythematous macules, papules, and reticulate hyperpigmentation in flexural areas. A distinct atypical variant exists, which features brown macules predominantly on the trunk, lower limbs,
[...] Read more.
Galli–Galli disease (GGD) is a rare genodermatosis that exhibits autosomal dominant inheritance with variable penetrance. GGD typically manifests with erythematous macules, papules, and reticulate hyperpigmentation in flexural areas. A distinct atypical variant exists, which features brown macules predominantly on the trunk, lower limbs, and extremities, with a notable absence of the hallmark reticulated hyperpigmentation in flexural areas. This review includes a detailed literature search and examines cases since GGD’s first description in 1982. It aims to synthesize the current knowledge on GGD, covering its etiology, clinical presentation, histopathology, diagnosis, and treatment. A significant aspect of this review is the exploration of the genetic, histopathological, and clinical parallels between GGD and Dowling-Degos disease (DDD), which is another rare autosomal dominant genodermatosis, particularly focusing on their shared mutations in the KRT5 and POGLUT1 genes. This supports the hypothesis that GGD and DDD may be different phenotypic expressions of the same pathological condition, although they have traditionally been recognized as separate entities, with suprabasal acantholysis being a distinctive feature of GGD. Lastly, this review discusses the existing treatment approaches, underscoring the absence of established guidelines and the limited effectiveness of various treatments.
Full article
(This article belongs to the Section Clinico-Pathological Correlation in Dermatopathology)
►▼
Show Figures
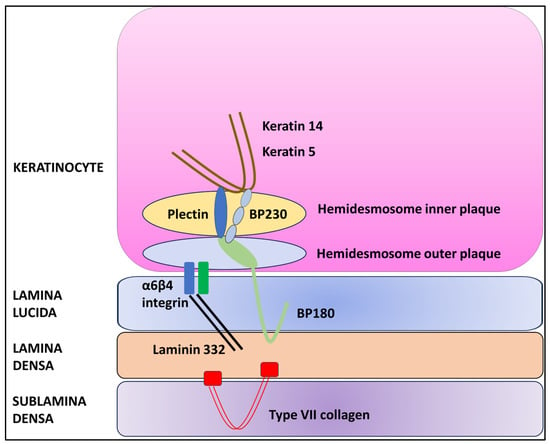
Figure 1
Open AccessReview
The Histopathology of Leg Ulcers
by
Amun Georg Hofmann, Julia Deinsberger, André Oszwald and Benedikt Weber
Dermatopathology 2024, 11(1), 62-78; https://doi.org/10.3390/dermatopathology11010007 - 29 Jan 2024
Abstract
►▼
Show Figures
Ulcerations of the lower extremities are a frequently encountered problem in clinical practice and are of significant interest in public health due to the high prevalence of underlying pathologies, including chronic venous disease, diabetes and peripheral arterial occlusive disease. However, leg ulcers can
[...] Read more.
Ulcerations of the lower extremities are a frequently encountered problem in clinical practice and are of significant interest in public health due to the high prevalence of underlying pathologies, including chronic venous disease, diabetes and peripheral arterial occlusive disease. However, leg ulcers can also present as signs and symptoms of various rare diseases and even as an adverse reaction to drugs. In such cases, correct diagnosis ultimately relies on histopathological examination. Apart from the macroscopic presentation, patient history and anatomic location, which are sometimes indicative, most ulcers have very distinct histopathological features. These features are found in different layers of the skin or even associated vessels. In this narrative review, we discuss and highlight the histopathological differences of several types of leg ulcers that can contribute to efficient and accurate diagnosis.
Full article
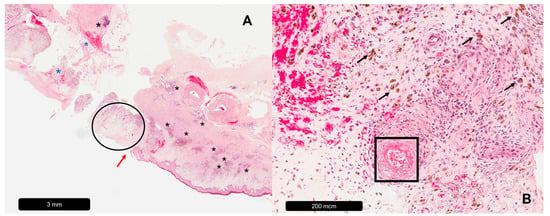
Figure 1
Open AccessReview
Direct Immunofluorescence of Skin and Oral Mucosa: Guidelines for Selecting the Optimum Biopsy Site
by
Muhammad N. Mahmood
Dermatopathology 2024, 11(1), 52-61; https://doi.org/10.3390/dermatopathology11010006 - 19 Jan 2024
Abstract
Direct immunofluorescence is a vital diagnostic test for assessing vesiculobullous disorders, vasculitides, and connective tissue diseases. It is a robust and valuable technique that offers essential diagnostic information for many critical dermatoses. Dermatopathologists depend heavily on the data obtained from direct immunofluorescence evaluation
[...] Read more.
Direct immunofluorescence is a vital diagnostic test for assessing vesiculobullous disorders, vasculitides, and connective tissue diseases. It is a robust and valuable technique that offers essential diagnostic information for many critical dermatoses. Dermatopathologists depend heavily on the data obtained from direct immunofluorescence evaluation to confirm final diagnoses. Selecting the most appropriate biopsy site is necessary for maximizing diagnostic accuracy, and the best site may vary depending on the clinical differential diagnosis. Inaccurate biopsy site selection can significantly impact the accuracy of the results. To optimize the use of direct immunofluorescence studies, this review provides helpful guidelines and some practical tips for selecting the best biopsy site.
Full article
Open AccessReview
Diagnosing Cutaneous Melanocytic Tumors in the Molecular Era: Updates and Review of Literature
by
Chelsea Huang, Tiffany Wing-See Lau and Bruce R. Smoller
Dermatopathology 2024, 11(1), 26-51; https://doi.org/10.3390/dermatopathology11010005 - 18 Jan 2024
Abstract
Over the past decade, molecular and genomic discoveries have experienced unprecedented growth, fundamentally reshaping our comprehension of melanocytic tumors. This review comprises three main sections. The first part gives an overview of the current genomic landscape of cutaneous melanocytic tumors. The second part
[...] Read more.
Over the past decade, molecular and genomic discoveries have experienced unprecedented growth, fundamentally reshaping our comprehension of melanocytic tumors. This review comprises three main sections. The first part gives an overview of the current genomic landscape of cutaneous melanocytic tumors. The second part provides an update on the associated molecular tests and immunohistochemical stains that are helpful for diagnostic purposes. The third section briefly outlines the diverse molecular pathways now utilized for the classification of cutaneous melanomas. The primary goal of this review is to provide a succinct overview of the molecular pathways involved in melanocytic tumors and demonstrate their practical integration into the realm of diagnostic aids. As the molecular and genomic knowledge base continues to expand, this review hopes to serve as a valuable resource for healthcare professionals, offering insight into the evolving molecular landscape of cutaneous melanocytic tumors and its implications for patient care.
Full article
(This article belongs to the Special Issue Histological Diagnostics of Malignant Melanoma: State of the Art and Perspectives)
►▼
Show Figures
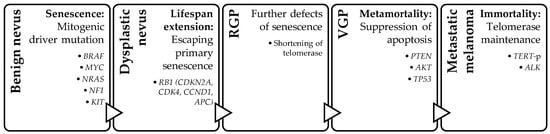
Figure 1
Open AccessCase Report
Giant Folliculosebaceous Cystic Hamartoma of the Face
by
Ramona Tasar, Melanie Peckruhn and Jörg Tittelbach
Dermatopathology 2024, 11(1), 19-25; https://doi.org/10.3390/dermatopathology11010004 - 31 Dec 2023
Abstract
►▼
Show Figures
Folliculosebaceous cystic hamartoma (FSCH) is a rare and benign form of cutaneous hamartomas. These skin lesions often lead to clinical and histopathological misdiagnosis due to their similarities to cutaneous lesions with overproduction of clustered sebaceous glands. Clinically, the lesions often present as solitary,
[...] Read more.
Folliculosebaceous cystic hamartoma (FSCH) is a rare and benign form of cutaneous hamartomas. These skin lesions often lead to clinical and histopathological misdiagnosis due to their similarities to cutaneous lesions with overproduction of clustered sebaceous glands. Clinically, the lesions often present as solitary, skin-colored, pedunculated warts to cauliflower-like, exophytic papules and nodules, usually with a diameter ranging 0.5–1.5 cm that rarely exceed 2 cm in size. Only a small number of giant variants are reported in the literature with a diameter in the range of 5–23 cm. The vast majority of the lesions appear in the central face and show a striking predilection for the nose, ears, and scalp, but also emerge on the nipples, extremities, and genitals. Histologically, the epithelial components of folliculosebaceous cystic hamartoma comprise dilated infundibular cystic proliferation with surrounding mesenchymal components, which commonly include fibroplasia and vascular and adipose tissue proliferation. These histological characteristics were coined by Kimura and colleagues (1991). To the best of our knowledge, our case represents the biggest variant of giant folliculosebaceous cystic hamartoma.
Full article
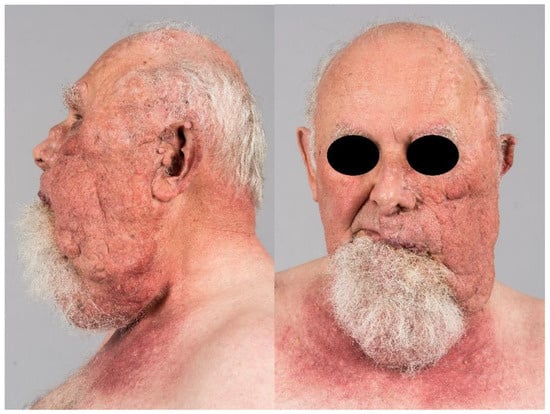
Figure 1
Open AccessCase Report
A Case of Pleomorphic Dermal Sarcoma: Giant Exophytic Tumor of the Medial Canthus
by
Rylee Moody, Kavita Darji, Tricia A. Missall, Peter Chow and Ramona Behshad
Dermatopathology 2024, 11(1), 13-18; https://doi.org/10.3390/dermatopathology11010003 - 29 Dec 2023
Abstract
We present the case of a 99-year-old Caucasian female who was referred for treatment of a painless, 8.0 cm × 7.8 cm exophytic, pedunculated, ulcerated tumor of the left medial canthus. Pathology showed spindled, oval, and polygonal cells with pleomorphic nuclei. Many multinuclear
[...] Read more.
We present the case of a 99-year-old Caucasian female who was referred for treatment of a painless, 8.0 cm × 7.8 cm exophytic, pedunculated, ulcerated tumor of the left medial canthus. Pathology showed spindled, oval, and polygonal cells with pleomorphic nuclei. Many multinuclear giant cells and mitotic figures were also noted. The tumor was highlighted with CD10, showed focal positivity with actin, desmin, and CD68, and had increased Ki67 immunohistochemical staining. The tumor was negative for pancytokeratin, CK5/6, p63, MART-1/MelanA, S100, Sox10, p40, CD34, and CD23. Based on clinicopathologic correlation, the diagnosis of pleomorphic dermal sarcoma (PDS) was made. Pleomorphic dermal sarcoma (PDS) refers to a deep, histologically high-grade tumor that often resembles other tumors clinically and histologically. As PDS is frequently aggressive and related to adverse outcomes, it is important to recognize its distinguishing features in comparison to other similar entities, including atypical fibroxanthoma (AFX) and pleomorphic leiomyosarcoma (PLMS). To our knowledge, there is only one other reported case in the literature of PDS occurring on the eye. By reviewing and understanding characteristic etiologies, locations of presentation, histopathological features, and management techniques, pathologists can make a more accurate diagnosis and dermatologists can provide more effective patient care in a timely manner.
Full article
(This article belongs to the Special Issue Educational Case Reports in Dermatopathology)
►▼
Show Figures
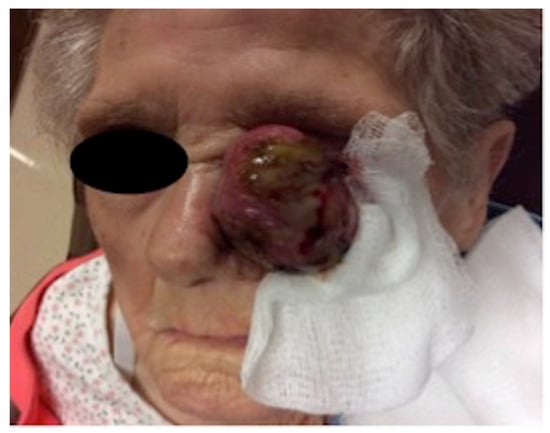
Figure 1
Open AccessCase Report
Perforating Fibrous Histiocytoma Mimicking Keratoacanthoma: A Case Report
by
Alina Lungu, Aurélie Hsieh, Gürkan Kaya and Sébastien Menzinger
Dermatopathology 2024, 11(1), 8-12; https://doi.org/10.3390/dermatopathology11010002 - 25 Dec 2023
Abstract
A 31-year-old male presented with a firm, well-demarcated, erythematous, crateriform, and ulcerated nodule in the left lumbar region, which persisted for 3 months. Clinically, a keratoacanthoma was suspected. The histological analysis was consistent with perforating fibrous histiocytoma, a rare histopathologic variant of fibrous
[...] Read more.
A 31-year-old male presented with a firm, well-demarcated, erythematous, crateriform, and ulcerated nodule in the left lumbar region, which persisted for 3 months. Clinically, a keratoacanthoma was suspected. The histological analysis was consistent with perforating fibrous histiocytoma, a rare histopathologic variant of fibrous histiocytoma. To our knowledge, this is the third case reported in the literature.
Full article
(This article belongs to the Section Clinico-Pathological Correlation in Dermatopathology)
►▼
Show Figures
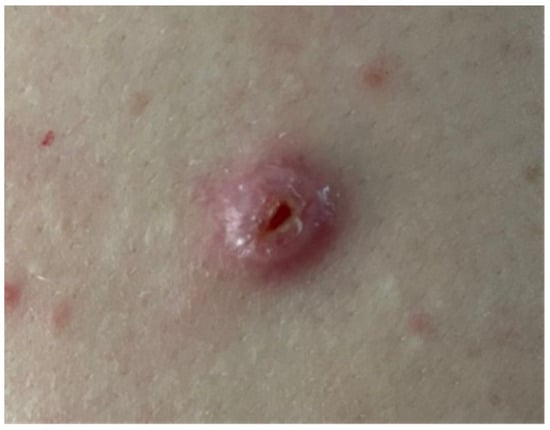
Figure 1
Open AccessCommunication
Claudin-4 Upregulation in Acantholytic and Autoimmune-Mediated Bullous Disorders
by
Chau M. Bui, Huy G. Vuong, Minh-Khang Le, Kristin J. Rybski, Hatice B. Zengin, Haiming Tang and Bruce R. Smoller
Dermatopathology 2024, 11(1), 1-7; https://doi.org/10.3390/dermatopathology11010001 - 21 Dec 2023
Abstract
►▼
Show Figures
Claudin-4 is a key component of tight junctions, which play an important role in the formation of the epidermal barrier by forming a circumferential network in the granular layer that serves as a gatekeeper of the paracellular pathway. The aim of this study
[...] Read more.
Claudin-4 is a key component of tight junctions, which play an important role in the formation of the epidermal barrier by forming a circumferential network in the granular layer that serves as a gatekeeper of the paracellular pathway. The aim of this study is to illustrate claudin-4 immunohistochemical staining patterns of different blistering disorders. We collected 35 cases, including two Hailey–Hailey disease, one Darier disease, three Grover disease, one acantholytic acanthoma, two warty dyskeratoma, 11 pemphigus vulgaris (PV) including six mucosal PV, and two pemphigus foliaceus. For comparison, we included five cases of normal skin, five eczema, and three bullous pemphigoid cases. Claudin-4 demonstrated weak-to-moderate expression in keratinocytes located in the stratum granulosum, keratinocytes surrounding hair follicles, and adnexal glands. Further, claudin-4 exhibited moderate-to-strong membranous staining in disrupted keratinocytes surrounding and within the acantholytic and bullous areas in 16/22 of the acantholytic cases (not seen in the six cases of mucosal PV) and all three bullous pemphigoids. This finding suggests that claudin-4 is upregulated in these conditions, which may be a compensatory response to the disrupted barrier function. This finding could shed light on the molecular mechanisms underlying disrupted barrier function in blistering disorders, independent of the specific underlying disease mechanism.
Full article
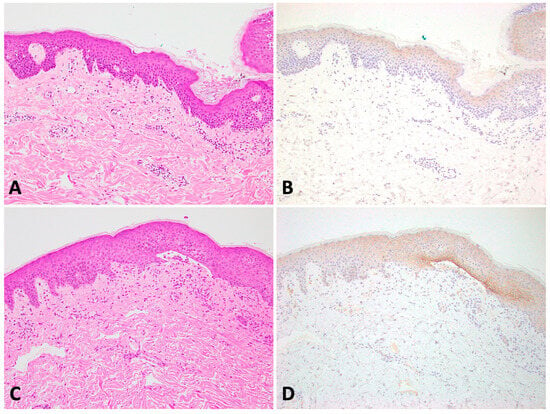
Figure 1
Open AccessCase Report
Dermatomyositis with Eosinophils
by
Isabella I. Sanchez, Henry O. Herrera, Ashley Elsensohn, Bonnie A. Lee and Christina N. Kraus
Dermatopathology 2023, 10(4), 310-317; https://doi.org/10.3390/dermatopathology10040039 - 21 Nov 2023
Abstract
Dermatomyositis is an idiopathic inflammatory myopathy that often presents with symmetric proximal skeletal muscle weakness and characteristic skin findings. Typical skin biopsy findings include vacuolar changes of the basal layer, increased dermal mucin, and a predominantly lymphocytic infiltrate. We report a case of
[...] Read more.
Dermatomyositis is an idiopathic inflammatory myopathy that often presents with symmetric proximal skeletal muscle weakness and characteristic skin findings. Typical skin biopsy findings include vacuolar changes of the basal layer, increased dermal mucin, and a predominantly lymphocytic infiltrate. We report a case of dermatomyositis presenting as intensely pruritic papules and plaques, with initial histopathology being atypical of dermatomyositis due to the presence of eosinophils. The initial biopsy demonstrated a superficial dermatitis with eosinophils, initially thought to represent a drug eruption. A second biopsy of the same cutaneous manifestation was performed at a later time given high clinical suspicion for dermatomyositis and demonstrated a more classic vacuolar interface dermatitis with increased mucin and an absence of eosinophils. Notably, increased pruritus was specifically associated with the lesion that demonstrated tissue eosinophilia. The case illustrates the importance of considering tissue eosinophilia in the histologic presentation of dermatomyositis.
Full article
(This article belongs to the Special Issue Educational Case Reports in Dermatopathology)
►▼
Show Figures
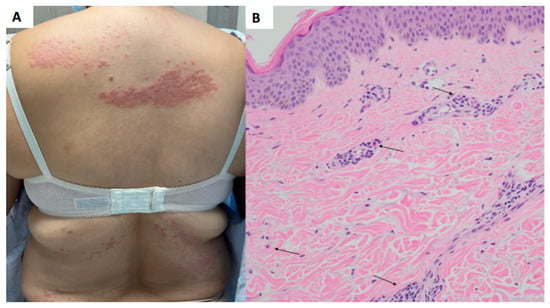
Figure 1
Open AccessCommunication
Folliculotropic Mycosis Fungoides Is Associated with Decreased PD1 Staining Compared with Classic Mycosis Fungoides
by
Haiming Tang, Kristin J. Rybski, Yi Luan and Bruce R. Smoller
Dermatopathology 2023, 10(4), 303-309; https://doi.org/10.3390/dermatopathology10040038 - 23 Oct 2023
Abstract
Programmed cell death protein 1 (PD-1) plays a pivotal role in immune system regulation, with its expression levels linked to malignancy prognosis. However, existing reports on PD-1 staining in mycosis fungoides (MF) present conflicting findings, and little attention has been given to PD-1
[...] Read more.
Programmed cell death protein 1 (PD-1) plays a pivotal role in immune system regulation, with its expression levels linked to malignancy prognosis. However, existing reports on PD-1 staining in mycosis fungoides (MF) present conflicting findings, and little attention has been given to PD-1 staining in different MF variants. To address this, we conducted a retrospective study, employing immunohistochemistry to examine PD-1 expression in cases of folliculotropic MF and non-folliculotropic MF. We analyzed 24 cases of folliculotropic MF and 18 cases of non-folliculotropic MF, and recorded both the percentage of PD-1-labeled tumor cells and the intensity score (negative, weak, medium, or strong). Our results revealed significant disparity in PD-1 labeling between patch/plaque MF and folliculotropic MF (p = 0.028). Non-folliculotropic MF exhibited higher PD-1 labeling in tumor cells (58.3%) compared to folliculotropic MF (40.2%). Notably, there was no significant difference in PD-1 staining between folliculotropic MF and non-folliculotropic MF when both were in the early stage/indolent disease category. However, when considering the tumor stage, folliculotropic MF exhibited PD-1 staining in tumor cells at a rate of 21.1%, while non-folliculotropic MF showed PD-1 staining in tumor cells at a rate of 46.6% (p = 0.005). Additionally, among folliculotropic MF cases, 13 out of 24 cases displayed differing PD-1 expression patterns between epidermal and dermal components, with preserved PD-1 staining in the epidermal component and loss of staining in the dermal component. Furthermore, consistent with the prior literature, tumor cells with large cell transformations exhibited significantly lower PD-1 labeling (p = 0.017). Our findings showcase the unique PD-1 staining patterns in MF.
Full article
(This article belongs to the Section Clinico-Pathological Correlation in Dermatopathology)
►▼
Show Figures
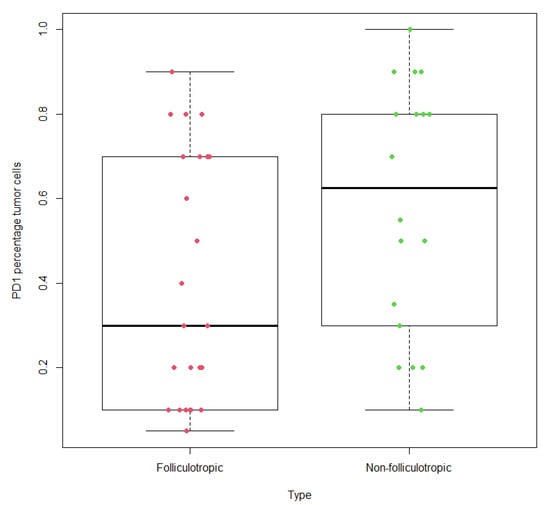
Figure 1
Open AccessCommunication
The Effect of Bacillus coagulans Induced Interactions among Intestinal Bacteria, Metabolites, and Inflammatory Molecules in Improving Natural Skin Aging
by
Keiichi Hiramoto, Sayaka Kubo, Keiko Tsuji, Daijiro Sugiyama, Yasutaka Iizuka and Hideo Hamano
Dermatopathology 2023, 10(4), 287-302; https://doi.org/10.3390/dermatopathology10040037 - 28 Sep 2023
Cited by 1
Abstract
Background: Lactic acid bacteria consumption serves several health benefits to humans. However, their effect on natural skin aging is still unclear. Methods: This study examined the effects of skin naturalization (particularly skin drying) by administering a spore-bearing lactic acid bacteria (Bacillus coagulans
[...] Read more.
Background: Lactic acid bacteria consumption serves several health benefits to humans. However, their effect on natural skin aging is still unclear. Methods: This study examined the effects of skin naturalization (particularly skin drying) by administering a spore-bearing lactic acid bacteria (Bacillus coagulans) in mice for 2 years. Results: B. coagulans administration improved the natural skin of mice and significantly increased proportions of the genera Bacteroides and Muribaculum, among other intestinal bacteria. As metabolites, increases in nicotinic acid, putrescin, and pantothenic acid levels and a decrease in choline levels were observed. Increased hyaluronic acid, interleukin-10, and M2 macrophage levels indicate aging-related molecules in the skin. Intestinal permeability was also suppressed. Thus, these changes together improved natural skin aging. Conclusions: This study revealed that B. coagulans administration improved the natural skin aging in mice. This enhancement might be induced by the interaction of alterations in intestinal flora, metabolites, or inflammatory substances.
Full article
(This article belongs to the Section Experimental Dermatopathology)
►▼
Show Figures
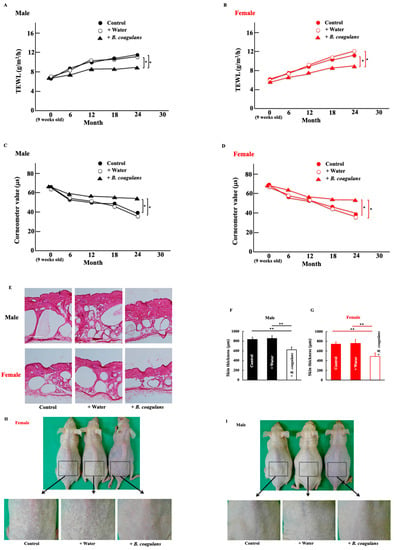
Figure 1
Open AccessCase Report
Lichen Planus Pigmentosus with True Melanocytic Nests: A Case Report with a Comprehensive Literature Review
by
Antonio Podo Brunetti, Gianmarco Diego Bigotto, Giorgio Stabile, Valentina Caputo, Lucia Brambilla, Stefania Guida and Franco Rongioletti
Dermatopathology 2023, 10(3), 281-286; https://doi.org/10.3390/dermatopathology10030036 - 8 Sep 2023
Abstract
Lichen Planus Pigmentosus (LPP) is an uncommon variant of lichen planus characterized by the development of dark greyish-brown macules and patches primarily affecting sun-exposed areas. Histologically, it presents with lichenoid interface dermatitis with many melanophages. In select cases, the presence of melanocytic nests
[...] Read more.
Lichen Planus Pigmentosus (LPP) is an uncommon variant of lichen planus characterized by the development of dark greyish-brown macules and patches primarily affecting sun-exposed areas. Histologically, it presents with lichenoid interface dermatitis with many melanophages. In select cases, the presence of melanocytic nests or pseudomelanocytic nests within LPP lesions has been documented, posing a diagnostic challenge. We present a detailed case report of a 32-year-old Eritrean woman with a longstanding history of hyperpigmented macules, alongside an in-depth review of the existing literature on lichenoid dermatoses featuring melanocytic or pseudomelanocytic nests. This paper delves into the clinical presentation, histopathological features, differential diagnosis, and potential mechanisms underlying this intriguing phenomenon.
Full article
(This article belongs to the Section Clinico-Pathological Correlation in Dermatopathology)
►▼
Show Figures
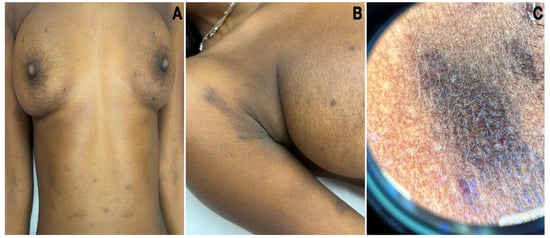
Figure 1
Open AccessReview
Endocrine Mucin-Producing Sweat Gland Carcinoma: Case Presentation with a Comprehensive Review of the Literature
by
Gerardo Cazzato, Emilio Bellitti, Irma Trilli, Anna Colagrande, Nicoletta Sgarro, Vincenza Sara Scarcella, Teresa Lettini, Giuseppe Ingravallo, Domenico Piscitelli, Leonardo Resta and Lucia Lospalluti
Dermatopathology 2023, 10(3), 266-280; https://doi.org/10.3390/dermatopathology10030035 - 1 Sep 2023
Cited by 1
Abstract
►▼
Show Figures
(1) Background: Endocrine Mucin-Producing Sweat Gland Carcinoma (EMPSGC) is a rare, low-grade, neuroendocrine-differentiated, cutaneous adnexal tumor, officially recognized by the World Health Organization (WHO) Skin Tumors Classification in 2018 as a separate entity and homologue of endocrine ductal carcinoma in situ (eDCIS)/solid papillary
[...] Read more.
(1) Background: Endocrine Mucin-Producing Sweat Gland Carcinoma (EMPSGC) is a rare, low-grade, neuroendocrine-differentiated, cutaneous adnexal tumor, officially recognized by the World Health Organization (WHO) Skin Tumors Classification in 2018 as a separate entity and homologue of endocrine ductal carcinoma in situ (eDCIS)/solid papillary carcinoma of the breast. Although it is more frequent in the female sex, between 60 and 70 years old, in the peri-orbital region, EMPSGC has also been described in the male sex, in subjects under 60 and over 80, and in extra-eyelid localizations (cheek, temple, scalp), but also in extra-facial localizations (chest and scrotum). (2) Methods: We present the clinical case of a 71-year-old woman with an undated lesion of the scalp, which presented as a nodule, skin-colored, and 2.5 cm in maximum diameter. We also conduct a comprehensive literature review from 1997 to the end of 2022, consulting PubMed, Scopus, Web of Science (WoS), and Google Scholar using the following keywords: “Endocrine mucin-producing sweat gland carcinoma” and/or “EMPSGC” and/or “skin” and “cutaneous neoplasms”. In addition, we followed the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines. A total of 253 patients were recorded; 146 were females (57.7%) and 107 were males (42.2%). The vast majority of the lesions were in the eyelids (peri-ocular region), and only a minority of cases involved the cheeks, supra-auricular, retro-auricular, and occipital region, with very rare cases in the scalp, to which the present is also added. (4) Conclusions: The morphological and immunophenotypical features are essential both for the correct diagnosis and to be able to classify this lesion among the corresponding eDCIS/solid papillary carcinoma of the breast, with neuroendocrine differentiation. Recent papers have attempted to shed light on the molecular features of EMPSGC, and much remains to be conducted in the attempt to subtype the molecular profiles of these entities. Future studies with large case series, and especially with molecular biology techniques, will be needed to further add information about EMPSGC and its relationship in the PCMC spectrum.
Full article
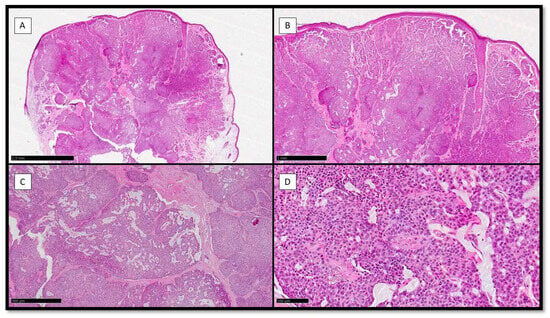
Figure 1
Highly Accessed Articles
Latest Books
E-Mail Alert
News
Topics

Conferences
Special Issues
Special Issue in
Dermatopathology
Tissue Scarring, Fibrosis and Regeneration
Guest Editor: Taihao QuanDeadline: 30 September 2024