Journal Description
European Burn Journal
European Burn Journal
(formerly European Journal of Burn Care) is an international, peer-reviewed, open access journal on burn care and burn prevention. The journal is owned by the European Burns Association (EBA) and is published quarterly online by MDPI.
- Open Access— free for readers, with article processing charges (APC) paid by authors or their institutions.
- High Visibility: indexed within ESCI (Web of Science), and other databases.
- Rapid Publication: manuscripts are peer-reviewed and a first decision is provided to authors approximately 26.7 days after submission; acceptance to publication is undertaken in 4.6 days (median values for papers published in this journal in the second half of 2023).
- Recognition of Reviewers: APC discount vouchers, optional signed peer review, and reviewer names published annually in the journal.
- Companion journal: Healthcare.
Latest Articles
An Optical Tomography-Based Score to Assess Pediatric Hand Burns
Eur. Burn J. 2024, 5(2), 155-165; https://doi.org/10.3390/ebj5020013 - 15 May 2024
Abstract
►
Show Figures
To define the morphologic pattern of pediatric hand burns as visualized via optical coherence tomography (OCT) and dynamic OCT (D-OCT). We designed a scoring system to assess the depths of burn wounds on pediatric hands and tested this score in our cohort of
[...] Read more.
To define the morphologic pattern of pediatric hand burns as visualized via optical coherence tomography (OCT) and dynamic OCT (D-OCT). We designed a scoring system to assess the depths of burn wounds on pediatric hands and tested this score in our cohort of children with burn injuries to the hand. Overall, 67 hand burns in 48 children (0–15 years) were prospectively examined. Scans were interpreted by two independent observers. Relevant OCT findings were surface irregularity, loss of epidermis, loss of dermal pattern (skin lines or papillary spots, loss of surface regularity and irregular vascular pattern of the plexus papillaris. Score values were calculated retrospectively. A score of 4 was associated with spontaneous healing without the need for skin grafting, with a positive predictive value of 97%. Deeper wounds with delayed healing and/or the need of skin grafting received a score of 5 or above, with an agreement of medical healing in 80% and a positive predictive value of 56%. OCT and D-OCT provide clinically useful additional information in cases of pediatric hand burns. The OCT burn score has the potential to support clinical decision making and, subsequently, improve clinical outcomes and shorten hospital stays.
Full article
Open AccessArticle
The Early Childhood Development of Pediatric Burn Patients
by
Maxime D. Cuijpers, Moniek Akkerman, Martin G. A. Baartmans, Paul P. M. van Zuijlen and Anouk Pijpe
Eur. Burn J. 2024, 5(2), 145-154; https://doi.org/10.3390/ebj5020012 - 14 May 2024
Abstract
►▼
Show Figures
Our study aimed to provide a description of the early childhood development of pediatric burn patients relative to Dutch reference values, using both pre- and post-burn data from the Dutch Development Instrument and the D-score. Data from the Dutch Development Instrument were
[...] Read more.
Our study aimed to provide a description of the early childhood development of pediatric burn patients relative to Dutch reference values, using both pre- and post-burn data from the Dutch Development Instrument and the D-score. Data from the Dutch Development Instrument were used to calculate the D-score and age-standardized D-score. Similar to a growth chart, the D-score was used to plot pediatric burn patients’ development relative to Dutch reference values for their age. Pediatric burn patients’ (n = 38) median age at the time of injury was 1.0 (1.0–2.0) years old. Burn size ranged from 1.0% to 36.0% of the total body surface area. Ninety-five percent (± 6.0%) of pediatric burn patients passed each of the age-appropriate developmental milestones at the target age. The mean age-standardized D-score was just above the Dutch average (+0.49 SD [0.18, 0.80]) and did not vary depending on sex (p = 0.06) or burn size (p = 0.41). In conclusion, among pediatric patients aged up to two-and-a-half years old, with non-full thickness burns, development was on track relative to the Dutch reference values. Our findings offer valuable first insights into the early childhood development of pediatric burn patients and may alleviate some parental concerns.
Full article

Figure 1
Open AccessArticle
Acute Surgical and Rehabilitation Management of Complex Hand Burns in Combat Casualties
by
Jill M. Cancio, Jonathan B. Lundy and Leopoldo C. Cancio
Eur. Burn J. 2024, 5(2), 126-144; https://doi.org/10.3390/ebj5020011 - 5 May 2024
Abstract
►▼
Show Figures
Burns are inevitable in modern warfare and have comprised between 5% and 20% of battlefield injuries. Involvement of the hands is the leading cause of postburn functional impairment. The purpose of this paper is to provide guidance on aspects of care necessary for
[...] Read more.
Burns are inevitable in modern warfare and have comprised between 5% and 20% of battlefield injuries. Involvement of the hands is the leading cause of postburn functional impairment. The purpose of this paper is to provide guidance on aspects of care necessary for the management of complex hand burns in a battlefield setting. Proper assessment and establishment of a comprehensive plan of care at the onset of injury help to ensure optimal functional outcomes in hand function. Basic treatment principles for the acutely burned hand include edema management; early wound coverage, including excision of the burn and skin grafting; early and aggressive hand therapy; and burn-scar contracture mitigation strategies.
Full article
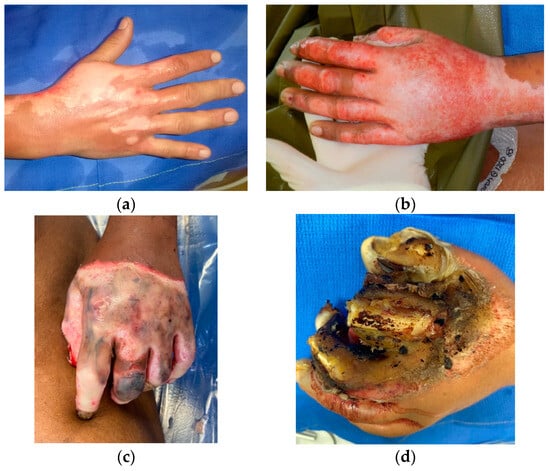
Figure 1
Open AccessArticle
Factors Associated with Self-Reported Voice Change in the Hospitalized Burn Population: A Burn Model System National Database Study
by
Kaitlyn L. Chacon, Edward Santos, Kara McMullen, Lauren J. Shepler, Carla Tierney-Hendricks, Audra T. Clark, Chiaka Akarichi, Haig A. Yenikomshian, Caitlin M. Orton, Colleen M. Ryan and Jeffrey C. Schneider
Eur. Burn J. 2024, 5(2), 116-125; https://doi.org/10.3390/ebj5020010 - 30 Apr 2024
Abstract
►▼
Show Figures
Voice plays a prominent role in verbal communication and social interactions. Acute burn care often includes intubation, mechanical ventilation, and tracheostomy, which could potentially impact voice quality. However, the issue of long-term dysphonia remains underexplored. This study investigates long-term self-reported voice changes in
[...] Read more.
Voice plays a prominent role in verbal communication and social interactions. Acute burn care often includes intubation, mechanical ventilation, and tracheostomy, which could potentially impact voice quality. However, the issue of long-term dysphonia remains underexplored. This study investigates long-term self-reported voice changes in individuals with burn injuries, focusing on the impact of acute burn care interventions. Analyzing data from a multicenter longitudinal database (2015–2023), self-reported vocal changes were examined at discharge and 6, 12, 24, and 60 months after injury. Out of 582 participants, 65 reported voice changes at 12 months. Changes were prevalent at discharge (16.4%) and persisted over 60 months (11.6–12.7%). Factors associated with voice changes included flame burn, inhalation injury, tracheostomy, outpatient speech-language pathology, head/neck burn, larger burn size, mechanical ventilation, and more ventilator days (p < 0.001). For those on a ventilator more than 21 days, 48.7% experience voice changes at 12 months and 83.3% had received a tracheostomy. The regression analysis demonstrates that individuals that were placed on a ventilator and received a tracheostomy were more likely to report a voice change at 12 months. This study emphasizes the need to understand the long-term voice effects of intubation and tracheostomy in burn care.
Full article
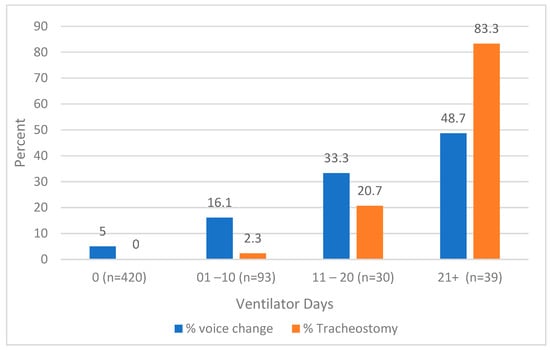
Figure 1
Open AccessArticle
Nonsteroidal Anti-Inflammatory Drugs Decrease Coagulopathy Incidence in Severe Burn Patients
by
Lyndon Huang, Kassandra Corona, Kendall Wermine, Elvia Villarreal, Giovanna De La Tejera, Phillip Howard Keys, Alen Palackic, Amina El Ayadi, George Golovko, Steven E. Wolf and Juquan Song
Eur. Burn J. 2024, 5(2), 104-115; https://doi.org/10.3390/ebj5020009 - 28 Apr 2024
Abstract
►▼
Show Figures
The study investigated the impact of nonsteroidal anti-inflammatory drugs (NSAIDs) on burn-induced coagulopathy in severely burned patients. Patients with a greater than 20% TBSA were identified in the TriNetX research network and categorized into receiving or not receiving NSAIDs in the first week
[...] Read more.
The study investigated the impact of nonsteroidal anti-inflammatory drugs (NSAIDs) on burn-induced coagulopathy in severely burned patients. Patients with a greater than 20% TBSA were identified in the TriNetX research network and categorized into receiving or not receiving NSAIDs in the first week after the burn. The statistical significance of the rate of burn-induced coagulopathy, mortality and sepsis in the week following injury was analysed. We observed 837 severely burned patients taking NSAIDS during the week following the burn and 1036 patients without. After matching for age, gender and race, the risk of burn-induced coagulopathy significantly decreased (p < 0.0001) in patients taking NSAIDs (17.7%) compared to those without (32.3%). Patients taking NSAIDs were also less likely to develop sepsis (p < 0.01) and thrombocytopenia (p < 0.001) or die the week following injury (p < 0.0001). In conclusion, the early protective effects of NSAIDs at reducing the risk of coagulopathy as well as sepsis and mortality occur during the acute phase of burns.
Full article
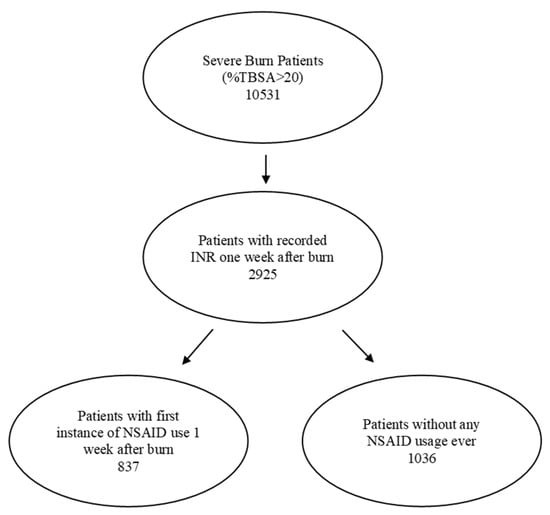
Figure 1
Open AccessArticle
Development and Testing of the Aftercare Problem List, a Burn Aftercare Screening Instrument
by
Nancy E. E. Van Loey, Elise Boersma-van Dam, Anita Boekelaar, Anneke van de Steenoven, Alette E. E. de Jong and Helma W. C. Hofland
Eur. Burn J. 2024, 5(2), 90-103; https://doi.org/10.3390/ebj5020008 - 29 Mar 2024
Abstract
A growing interest in person-centered care from a biopsychosocial perspective has led to increased attention to structural screening. The aim of this study was to develop an easy-to-comprehend screening instrument using single items to identify a broad range of health-related problems in adult
[...] Read more.
A growing interest in person-centered care from a biopsychosocial perspective has led to increased attention to structural screening. The aim of this study was to develop an easy-to-comprehend screening instrument using single items to identify a broad range of health-related problems in adult burn survivors. This study builds on earlier work regarding content generation. Focus groups and expert meetings with healthcare providers informed content refinement, resulting in the Aftercare Problem List (APL). The instrument consists of 43 items divided into nine health domains: scars, daily life functioning, scars treatment, body perceptions, stigmatization, intimacy, mental health, relationships, financial concerns, and a positive coping domain. The APL also includes a Distress Thermometer and a question inquiring about preference to discuss the results with a healthcare provider. Subsequently, the APL was completed by 102 outpatients. To test face validity, a linear regression analysis showed that problems in three health domains, i.e., scars, mental health, and body perceptions, were significantly related to higher distress. Qualitative results revealed that a minority found the items difficult which led to further adjustment of the wording and the addition of illustrations. In summation, this study subscribes to the validity of using single items to screen for burn-related problems.
Full article
(This article belongs to the Special Issue Person-Centered and Family-Centered Care Following Burn Injuries)
►▼
Show Figures

Figure 1
Open AccessArticle
Parental Stress and Child Quality of Life after Pediatric Burn
by
Dinithi Atapattu, Victoria M. Shoesmith, Fiona M. Wood and Lisa J. Martin
Eur. Burn J. 2024, 5(2), 77-89; https://doi.org/10.3390/ebj5020007 - 27 Mar 2024
Abstract
Parents’ emotions after their child’s burn might be influenced by the injury circumstances or demographic characteristics of the patient and family. Parents’ post-traumatic stress symptoms and their child’s distress may interact and affect emotional states. The psychosocial outcomes of parents were measured using
[...] Read more.
Parents’ emotions after their child’s burn might be influenced by the injury circumstances or demographic characteristics of the patient and family. Parents’ post-traumatic stress symptoms and their child’s distress may interact and affect emotional states. The psychosocial outcomes of parents were measured using the Impact of Event Scale-Revised, the CARe Burn Scale, and the Post-traumatic Growth Inventory-Brief. The psychosocial quality of life outcomes of the pediatric burn patients were measured using the Pediatric Quality of Life Inventory (PedsQL). Regression analysis was used to assess the relationship between patient psychosocial quality of life and the related parent scores. A total of 48 patients and parents participated, with 36 giving full data at 12 months. Parental post-traumatic stress symptoms were initially high, settling by six months, although outliers remained. Parents reported higher IESR scores if their child was female, if they felt helpless at the time of the incident, and if a language other than English was spoken in the home. Parents’ scores of their child’s psychosocial function were similar to their child’s self-scores. Parents who perceived poorer emotional functioning in their child reported higher IESR scores.
Full article
(This article belongs to the Special Issue Person-Centered and Family-Centered Care Following Burn Injuries)
►▼
Show Figures

Figure 1
Open AccessReview
Extracorporeal Organ Support for Burn-Injured Patients
by
Garrett W. Britton, Amanda R. Keith, Barret J. Halgas, Joshua M. Boster, Nicholas S. Niazi, Kevin K. Chung and Leopoldo C. Cancio
Eur. Burn J. 2024, 5(2), 66-76; https://doi.org/10.3390/ebj5020006 - 25 Mar 2024
Abstract
As mortality relating to severe acute burn injury improves, patients are surviving longer into the critical care phase, which is commonly complicated by multisystem organ failure. Extracorporeal organ support (ECOS) represents a set of potential therapeutic technologies for managing patients with organ-specific complications.
[...] Read more.
As mortality relating to severe acute burn injury improves, patients are surviving longer into the critical care phase, which is commonly complicated by multisystem organ failure. Extracorporeal organ support (ECOS) represents a set of potential therapeutic technologies for managing patients with organ-specific complications. This article provides a comprehensive review of the existing literature, focusing on the use of continuous kidney replacement therapy, extracorporeal membrane oxygenation, extracorporeal carbon dioxide removal, and extracorporeal blood purification. Though promising, many of these technologies are in the early phases of implementation and are restricted to well-resourced medical systems, limiting their use in large scale casualty and austere scenarios.
Full article
(This article belongs to the Special Issue Burn Injuries Associated with Wars and Disasters)
Open AccessReview
Burn Wound Care Strategies for the Battlefield and Austere Settings
by
Sarah Shingleton, Jared Folwell, Ian Jones, Michael Gleason and Alicia Williams
Eur. Burn J. 2024, 5(1), 49-65; https://doi.org/10.3390/ebj5010005 - 23 Feb 2024
Abstract
Burns are commonly encountered in the battlefield environment; however, the availability of burn expertise and specialized supplies is variable. Initial burn care should remain focused on cooling the burn, preventing hypothermia, basic wound cleansing, and evacuation. Key ongoing burn wound management principles include
[...] Read more.
Burns are commonly encountered in the battlefield environment; however, the availability of burn expertise and specialized supplies is variable. Initial burn care should remain focused on cooling the burn, preventing hypothermia, basic wound cleansing, and evacuation. Key ongoing burn wound management principles include wound debridement, accurate burn size and depth estimation, wound care, ongoing wound evaluation, and treatment of suspected Gram-negative wound infection. Operative management should be limited to urgent procedures, and definitive burn management should be performed only after evacuation to a higher level of care. Flexibility, creativity, and the ability to adapt care to the tactical environment are key to the successful management of burn injuries in battlefield and austere settings.
Full article
(This article belongs to the Special Issue Burn Injuries Associated with Wars and Disasters)
Open AccessFeature PaperArticle
Comparison of Clinical Estimation and Stereophotogrammic Instrumented Imaging of Burn Scar Height and Volume
by
Shyla Kajal Bharadia and Vincent Gabriel
Eur. Burn J. 2024, 5(1), 38-48; https://doi.org/10.3390/ebj5010004 - 12 Feb 2024
Abstract
►▼
Show Figures
Descriptive clinical tools for characterizing burn scars are limited by between-user variability and unknown sensitivity to change over time. We previously described preclinical assessment of stereophotogrammetry as a valid measure of burn-related scars. Here, we compared the estimated vs. instrumented measurements of maximum
[...] Read more.
Descriptive clinical tools for characterizing burn scars are limited by between-user variability and unknown sensitivity to change over time. We previously described preclinical assessment of stereophotogrammetry as a valid measure of burn-related scars. Here, we compared the estimated vs. instrumented measurements of maximum height and total positive volume of 26 burn scars. The burn scars were imaged with the QuantifiCare LifeViz Micro 3D camera. Three experienced wound care therapists first estimated, then measured using 3D Track software, the imaged scars’ height and volume. Two-factor analysis without replication was performed to calculate intraclass correlation coefficients (ICCs) between assessors’ estimated scar height and volume, and measured height and volume. Two-sided Wilcoxon tests were performed comparing the mean estimated height and volume with the estimated and measured outputs. The estimated scar height’s ICC was 0.595, and for volume, it was 0.531. The measured scar height’s ICC was 0.933 and for volume, it was 0.890. The estimated and measured volume were significantly different (z = −2.87, p = 0.041), while the estimated and measured height were not (z = −1.39, p = 0.161). Stereophotogrammic measurement of scar height and volume is more reliable than clinical photograph assessment. Stereophotogrammetry should be utilized when assessing burn scar height and volume, rather than subjective estimates from clinical scar tools.
Full article

Figure 1
Open AccessReview
Enteral Resuscitation: A Field-Expedient Treatment Strategy for Burn Shock during Wartime and in Other Austere Settings
by
Ian F. Jones, Kiran Nakarmi, Hannah B. Wild, Kwesi Nsaful, Kajal Mehta, Raslina Shrestha, Daniel Roubik and Barclay T. Stewart
Eur. Burn J. 2024, 5(1), 23-37; https://doi.org/10.3390/ebj5010003 - 18 Jan 2024
Abstract
Burn injuries are a constant threat in war. Aspects of the modern battlefield increase the risk of burn injuries and pose challenges for early treatment. The initial resuscitation of a severely burn-injured patient often exceeds the resources available in front-line medical facilities. This
[...] Read more.
Burn injuries are a constant threat in war. Aspects of the modern battlefield increase the risk of burn injuries and pose challenges for early treatment. The initial resuscitation of a severely burn-injured patient often exceeds the resources available in front-line medical facilities. This stems mostly from the weight and volume of the intravenous fluids required. One promising solution to this problem is enteral resuscitation with an oral rehydration solution. In addition to being logistically easier to manage, enteral resuscitation may be able to mitigate secondary injuries to the gut related to burn shock and systemic immunoinflammatory activation. This has been previously studied in burn patients, primarily using electrolyte solutions, with promising results. Modern ORS containing sodium, potassium, and glucose in ratios that maximize gut absorption may provide additional benefits as a resuscitation strategy, both in terms of plasma volume expansion and protection of the barrier and immune functions of the gut mucosa. While enteral resuscitation is promising and should be used when other options are not available, further research is needed to refine an optimal implementation strategy.
Full article
(This article belongs to the Special Issue Burn Injuries Associated with Wars and Disasters)
►▼
Show Figures

Figure 1
Open AccessArticle
Combat and Operational Stress Control: Application in a Burn Center
by
Jill M. Cancio and Leopoldo C. Cancio
Eur. Burn J. 2024, 5(1), 12-22; https://doi.org/10.3390/ebj5010002 - 29 Dec 2023
Abstract
Occupational therapy has been integral to the holistic recovery of soldiers since its origin. The positive psychosocial and physiological effects of occupation-based interventions, fundamental to the profession, have long justified its relevance to the military. As such, occupational therapy has been written into
[...] Read more.
Occupational therapy has been integral to the holistic recovery of soldiers since its origin. The positive psychosocial and physiological effects of occupation-based interventions, fundamental to the profession, have long justified its relevance to the military. As such, occupational therapy has been written into US Army doctrine as an integral component of the Combat and Operational Stress Control (COSC) program. The focus of a COSC unit is to prevent, identify, reduce, and manage combat and operational stress reactions resulting from physical and mental stressors in a combat environment. COSC centers around the recognition and resolution of functional problems and the development of enhanced coping skills. Recognizing that burn patients are, like combatants, also at high risk of stress-related illness, we applied COSC concepts to peacetime burn care. In this paper we describe the theoretical basis for COSC in a burn center. The COSC model supports holistic, functional recovery of the burn casualty and can augment psychosocial recovery, particularly in times of limited resources.
Full article
Open AccessArticle
Pain Management during Bromelain-Based Enzymatic Debridement (NexoBrid®) in a USA Adult Burn Center
by
Martin R. Buta, Domenic Annand, Sarah Findeisen, Sean A. Hickey, Robert L. Sheridan, Jonathan S. Friedstat, John T. Schulz, Branko Bojovic, Edward A. Bittner and Jeremy Goverman
Eur. Burn J. 2024, 5(1), 1-11; https://doi.org/10.3390/ebj5010001 - 19 Dec 2023
Abstract
►▼
Show Figures
Outside the United States, bromelain-based enzymatic debridement (BBED) has become an effective tool for the removal of burn eschar. A primary concern with BBED is that it is a painful procedure requiring appropriate analgesia. The purpose of this study was to describe our
[...] Read more.
Outside the United States, bromelain-based enzymatic debridement (BBED) has become an effective tool for the removal of burn eschar. A primary concern with BBED is that it is a painful procedure requiring appropriate analgesia. The purpose of this study was to describe our experience using NexoBrid® (NXB), with a particular focus on pain management. We performed a retrospective review on all 32 adult burn patients enrolled at our institution as part of a multicenter phase 3 clinical trial (DETECT) or the expanded access treatment protocol (NEXT). All patients underwent BBED with NXB of acute deep partial- and full-thickness thermal burn wounds at a major burn center between November 2016 and February 2023. Thirty-two patients with an average age of 42.1 years (SD = 17.4, range 18–72) and an average TBSA of 6.3% (SD = 5.9, range 1–24.5) underwent a total of 33 BBED procedures. Only one patient required an additional NXB treatment, and all patients achieved >95% eschar removal. For pain control during debridement, seven patients required a local block (LB), nine a regional block (RB), and thirteen conscious sedation (CS). Three patients were intubated (INTB) for their burn injury prior to the procedure. There was no statistical difference in Numerical Pain Rating Scale (NPRS) scores during vs. before treatment or after vs. before treatment for all patients or when subdivided by BMI, race, TBSA, total area treated, and anesthetic type (LB, RB, and CS). With appropriate analgesia, the pain associated with BBED of acute deep partial- and full-thickness thermal burns is well tolerated.
Full article

Figure 1
Open AccessFeature PaperReview
War at Sea: Burn Care Challenges—Past, Present and Future
by
Matthew D. Tadlock, Theodore D. Edson, Jill M. Cancio, Dana M. Flieger, Aaron S. Wickard, Bailey Grimsley, Corey G. Gustafson, Jay A. Yelon, James C. Jeng and Jennifer M. Gurney
Eur. Burn J. 2023, 4(4), 605-630; https://doi.org/10.3390/ebj4040041 - 11 Dec 2023
Abstract
Throughout history, seafarers have been exposed to potential thermal injuries during naval warfare; however, injury prevention, including advances in personal protective equipment, has saved lives. Thankfully, burn injuries have decreased over time, which has resulted in a significant clinical skills gap. Ships with
[...] Read more.
Throughout history, seafarers have been exposed to potential thermal injuries during naval warfare; however, injury prevention, including advances in personal protective equipment, has saved lives. Thankfully, burn injuries have decreased over time, which has resulted in a significant clinical skills gap. Ships with only Role 1 (no surgical capability) assets have worse outcomes after burn injury compared to those with Role 2 (surgical capability) assets. To prepare for future burn care challenges during a war at sea, Military Medicine must re-learn the lessons of World War I and World War II. Burn injuries do not occur in isolation during war and are associated with concomitant traumatic injuries. To care for burn casualties at sea, there is an urgent need to increase the availability of whole blood and dried plasma, resuscitation fluids that were ubiquitous throughout the naval force during World War II for both hemorrhagic and burn shock resuscitation. Furthermore, those providing trauma care at sea require formal burn care training and skills sustainment experiences in the clinical management of Burn, Trauma, and Critical Care patients. While burn education, training, and experience must be improved, modern high-energy weapons systems and anti-ship ballistic missiles necessitate concurrent investments in prevention, countermeasures, and personal protective equipment to decrease the likelihood of burn injury and damage resulting from these attacks.
Full article
(This article belongs to the Special Issue Burn Injuries Associated with Wars and Disasters)
►▼
Show Figures

Figure 1
Open AccessArticle
Procalcitonin in the Post-Operative Burn Patient
by
Ludo Masole, Chikwendu J. Ede and Adelin Muganza
Eur. Burn J. 2023, 4(4), 596-604; https://doi.org/10.3390/ebj4040040 - 16 Nov 2023
Abstract
►▼
Show Figures
Serum procalcitonin (PCT) is a biomarker used to diagnose sepsis and infection. Following invasive bacterial infection, PCT is detectable in peripheral blood. The aim of our study was to determine if there is a relationship between serum PCT post-burn wound debridement and burn-related
[...] Read more.
Serum procalcitonin (PCT) is a biomarker used to diagnose sepsis and infection. Following invasive bacterial infection, PCT is detectable in peripheral blood. The aim of our study was to determine if there is a relationship between serum PCT post-burn wound debridement and burn-related sepsis. In total, 34 participants were recruited from 1 November 2019 to 31 July 2020. Serum PCT levels were drawn on days 0, 1, 2, and 3, with day 0 being the day of the surgery. Blood culture samples were drawn on days 0 and 3. Statistical analyses were performed using STATA©. Descriptive statistics were presented as the median for continuous data and frequencies for categorical data. A two-sample Wilcoxon–Mann–Whitney test was performed to assess the correlation between the PCT values and blood culture positivity. In all, 33 burn debridement procedures were completed, and 1 patient demised before surgery. The median age was 35.5 years; 61.8% were male. Four patients had comorbidities. There was a trend of higher PCT values from day 0 to day 3. The median PCT on day 0 was 3.30 µg/L (IQR 0.78–15.10), compared to day 3 PCT which was 5.15 µg/L (IQR 1.35–18.55). The median values for serum PCT for days 0 to 3 were above the normal threshold regardless of BC positivity. There was a statistically significant difference in the PCT levels between positive and negative BC, with a p value of 0.0087 for day 3 serum PCT. The findings indicate an association of a high serum PCT level with a positive blood culture in a burn patient post-debridement surgery. A higher numerical threshold/cut-off of serum PCT should be used for this cohort of patients, to aid in the diagnosis of sepsis. A cut-off value could not be determined due to the small sample size.
Full article
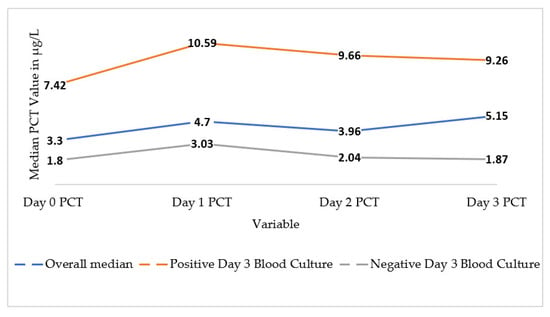
Figure 1
Open AccessReview
Management of Casualties from Radiation Events
by
Robert Alan Dent
Eur. Burn J. 2023, 4(4), 584-595; https://doi.org/10.3390/ebj4040039 - 14 Nov 2023
Cited by 1
Abstract
Radiation events such as nuclear war, nuclear reactor incidents, and the deployment of a radioactive dispersal device (dirty bomb) are all significant threats in today’s world. Each of these events would bring significant challenges to clinicians caring for patients with burns and traumatic
[...] Read more.
Radiation events such as nuclear war, nuclear reactor incidents, and the deployment of a radioactive dispersal device (dirty bomb) are all significant threats in today’s world. Each of these events would bring significant challenges to clinicians caring for patients with burns and traumatic injuries who are also contaminated or irradiated. The result of a nuclear exchange in a densely populated area could result in thousands of patients presenting with trauma, burns, and combined injury (trauma and burn in an irradiated patient). In this review, we will discuss the three major types of ionizing radiation: alpha, beta, and gamma, and their respective health hazards and biological effects. Additionally, we will discuss the types of burn injuries in a nuclear disaster, caring for the contaminated patient, and managing the combined injury of burn trauma with acute radiation syndrome. The reader will also be left with an understanding of how to prioritize lifesaving interventions, estimate the absorbed dose of radiation, and predict the onset of acute radiation syndrome. While some animal models for morbidity and mortality exist, there is limited modern day human data for patients with combined injury and burns associated with a nuclear disaster due to the infrequent nature of these events. It is extremely important to continue multidisciplinary research on the prevention of, preparedness for, and the response to nuclear events. Furthermore, continued exploration of novel treatments for radiation induced burns and the management of combined injury is necessary.
Full article
(This article belongs to the Special Issue Burn Injuries Associated with Wars and Disasters)
►▼
Show Figures

Figure 1
Open AccessReview
Pharmacologic Considerations for Antimicrobials and Anticoagulants after Burn Injury
by
Pranav Ravichandran and Kaitlin A. Pruskowski
Eur. Burn J. 2023, 4(4), 573-583; https://doi.org/10.3390/ebj4040038 - 10 Nov 2023
Cited by 1
Abstract
Derangements in pharmacokinetics and pharmacodynamics (PK/PD) of burn patients are poorly understood and lacking consistent data. This leads to an absence of consensus regarding pharmacologic management of burn patients, complicating their care. In order to effectively manage burn critical illness, knowledge of pharmacologic
[...] Read more.
Derangements in pharmacokinetics and pharmacodynamics (PK/PD) of burn patients are poorly understood and lacking consistent data. This leads to an absence of consensus regarding pharmacologic management of burn patients, complicating their care. In order to effectively manage burn critical illness, knowledge of pharmacologic parameters and their changes is necessary. It is also imperative that the clinician understands how these changes will affect drug dosing. A common practice is to increase antibiotic dosing and/or frequency; however, this may not be necessary and doses should be adjusted to patient- and drug-specific parameters. Additionally, monitoring assays for antibiotic levels as well as coagulation factors can be useful for adjusting dosages to best treat the patient. This review focuses on alterations in PK/PD as well as other physiologic changes after burn injury, with special reference to care in military and austere settings.
Full article
(This article belongs to the Special Issue Burn Injuries Associated with Wars and Disasters)
Open AccessReview
Burn Patient Perspectives on Disability Weights and the Philosophy of Disability: A Gap in the Literature
by
Paul Won, Karel-Bart Celie, Cindy Rutter, T. Justin Gillenwater and Haig A. Yenikomshian
Eur. Burn J. 2023, 4(4), 563-572; https://doi.org/10.3390/ebj4040037 - 9 Nov 2023
Cited by 1
Abstract
►▼
Show Figures
Background: Disability-adjusted life years (DALY) have a ubiquitous presence in academic global health, including attempts to understand the global burden of burn injuries. Objective: The present scoping review aimed to examine whether disability weights (DWs) were informed by burn patient perspectives and secondarily
[...] Read more.
Background: Disability-adjusted life years (DALY) have a ubiquitous presence in academic global health, including attempts to understand the global burden of burn injuries. Objective: The present scoping review aimed to examine whether disability weights (DWs) were informed by burn patient perspectives and secondarily to determine whether literature indicates which of the three most common philosophical models of disability best aligns with burn patient experiences. Methods: A review of six databases was conducted and The Critical Appraisal Skills Program (CASP) checklist was utilized. Results: Out of a total of 764 articles, zero studies solicited patient perspectives of DWs. Four articles contained data that could be extrapolated to patient perspectives on disability. All articles utilized semi-structured interviews of burn survivors and reported thematic elements including return to work, self-image, and social integration. Patients reported similar themes that burn injuries were disabling injuries and instrumentally detrimental, with modulation based on the patient’s social circumstances. Conclusions: This scoping review highlights a significant gap in literature. First, no studies were found directly investigating burn patient perspectives on burn DWs. Current DWs have been derived from expert opinions with limited input from patients. Second, the limited primary patient data gleaned from this review suggest patients consider their injuries as instrumentally detrimental, which aligns most closely with the welfarist view of disability. More explicit investigations into the philosophical model of disability best aligning with burn patient experiences are needed to ground the health economics of burns in sound theory.
Full article
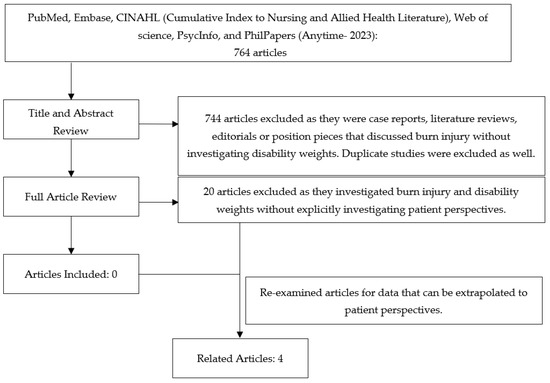
Figure 1
Open AccessSystematic Review
Efficacy and Complications Associated with Acellular Dermal Substitute Use in the Treatment of Acute Burns: A Systematic Review and Meta-Analysis
by
Isobel Press, Naiem Moiemen and Zubair Ahmed
Eur. Burn J. 2023, 4(4), 548-562; https://doi.org/10.3390/ebj4040036 - 23 Oct 2023
Cited by 1
Abstract
Over several decades, skin substitutes have become an essential tool in acute burn surgery, particularly in major burns, where scarce donor tissues can limit the availability of autografts. This systematic review aimed to assess the efficacy, complication rates, and long-term outcomes of acellular
[...] Read more.
Over several decades, skin substitutes have become an essential tool in acute burn surgery, particularly in major burns, where scarce donor tissues can limit the availability of autografts. This systematic review aimed to assess the efficacy, complication rates, and long-term outcomes of acellular dermal substitutes in acute burns and compare these to conventional skin grafting methods of coverage. A search of PubMed, Web of Science, and CENTRAL for appropriate randomized controlled trials (RCTs), non-randomized trials, and observational studies was conducted. Following screening, nine RCTs and seven observational studies fulfilled our inclusion and exclusion criteria. Our primary outcomes, which were graft take and incidence of infection, found no significant difference between the substitute and control procedures in a meta-analysis (p = 0.37 and p = 0.87, respectively). For our secondary outcomes, the studies were analyzed via narrative synthesis, which reported variable rates of graft loss and duration of acute hospital stay, from which definitive conclusions could not be drawn due to the heterogeneity in reporting. Despite a high risk of bias in the included studies, the evidence reviewed suggests that the treatment of an acute burn with a substitute may improve scar quality when compared to conventional grafting. This review therefore suggests that acellular dermal substitutes offer a viable method for staging the closure of deep partial- and full-thickness acute burns, although more robust RCTs with less heterogeneity are needed to support these conclusions.
Full article
(This article belongs to the Special Issue Epidermal and Dermal Skin Substitutes in Burn Care)
►▼
Show Figures
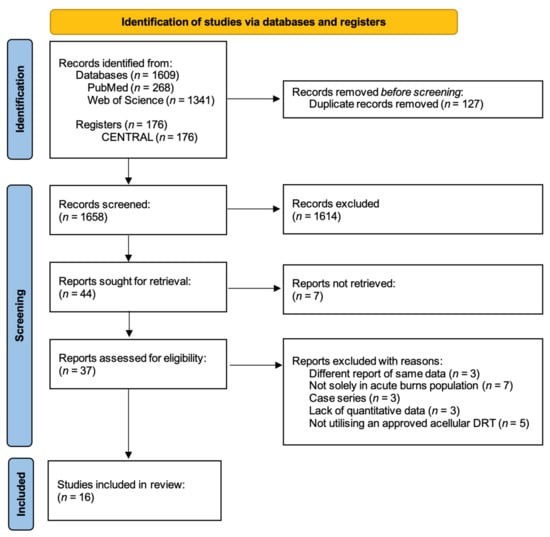
Figure 1
Open AccessFeature PaperReview
Nutrition Considerations for Burn Patients: Optimizing Recovery and Healing
by
Beth A. Shields and Asia M. Nakakura
Eur. Burn J. 2023, 4(4), 537-547; https://doi.org/10.3390/ebj4040035 - 13 Oct 2023
Cited by 1
Abstract
The hypermetabolic and hypercatabolic responses to severe burns put nutrition support at the forefront of treatments. When left untreated, severe weight loss, increased infection, and wound healing failure can occur. Enteral nutrition is the primary method of nutrition support in such patients. Meeting
[...] Read more.
The hypermetabolic and hypercatabolic responses to severe burns put nutrition support at the forefront of treatments. When left untreated, severe weight loss, increased infection, and wound healing failure can occur. Enteral nutrition is the primary method of nutrition support in such patients. Meeting caloric needs and a positive nitrogen balance are short-term goals of nutrition support, with long-term goals of minimizing lean body mass loss and maximizing wound healing. High-carbohydrate and low-fat nutrition received evidence from randomized controlled trials of aiding in decreasing pneumonia rates and was found to promote positive nitrogen balance, which lipids do not do. We go through the macronutrient and micronutrient needs of the burn patient as well as techniques for meeting these needs in the modern intensive care unit, with some discussion of alterations in these techniques that are required in the austere environment.
Full article
(This article belongs to the Special Issue Burn Injuries Associated with Wars and Disasters)
Highly Accessed Articles
Latest Books
E-Mail Alert
News
Topics

Conferences
Special Issues
Special Issue in
EBJ
Enhancing Burn Rehabilitation: Contemporary Improvements across the Spectrum of Influence
Guest Editors: Dale Edgar, Colleen Ryan, Marianne K. Nieuwenhuis, Ulrike Van Daele, Jill CancioDeadline: 1 September 2024
Special Issue in
EBJ
Long-Term Outcomes after Burn Injuries: Strategies to Optimize Recovery
Guest Editors: Nicole S. Gibran, Haig Yenikomshian, Gretchen Carrougher, Samuel MandellDeadline: 31 December 2024






