Journal Description
Advances in Respiratory Medicine
Advances in Respiratory Medicine
is an international, peer-reviewed, open access journal on respiratory medicine, covering allergology, oncology, immunology, and infectious diseases of the respiratory system. The journal is owned by the Polish Respiratory Society and is published bimonthly online by MDPI (since Volume 90, Issue 4 - 2022).
- Open Access— free for readers, with article processing charges (APC) paid by authors or their institutions.
- High Visibility: indexed within Scopus, ESCI (Web of Science), PubMed, MEDLINE, PMC, and other databases.
- Rapid Publication: manuscripts are peer-reviewed and a first decision is provided to authors approximately 25.9 days after submission; acceptance to publication is undertaken in 3.6 days (median values for papers published in this journal in the second half of 2023).
- Recognition of Reviewers: APC discount vouchers, optional signed peer review, and reviewer names published annually in the journal.
Impact Factor:
1.8 (2022);
5-Year Impact Factor:
1.6 (2022)
Latest Articles
Extracellular Water Ratio and Phase Angle as Predictors of Exacerbation in Chronic Obstructive Pulmonary Disease
Adv. Respir. Med. 2024, 92(3), 230-240; https://doi.org/10.3390/arm92030023 (registering DOI) - 31 May 2024
Abstract
Background: Chronic obstructive pulmonary disease (COPD), characterized by high-energy metabolism, often leads to malnutrition and is linked to exacerbations. This study investigates the association of malnutrition-related body composition and handgrip strength changes with exacerbation frequencies in COPD patients. Methods: We analyzed 77 acute
[...] Read more.
Background: Chronic obstructive pulmonary disease (COPD), characterized by high-energy metabolism, often leads to malnutrition and is linked to exacerbations. This study investigates the association of malnutrition-related body composition and handgrip strength changes with exacerbation frequencies in COPD patients. Methods: We analyzed 77 acute exacerbation COPD (AECOPD) patients and 82 stable COPD patients, categorized as frequent and infrequent exacerbators. Assessments included body composition, handgrip strength, nutritional risk, dyspnea scale, and COPD assessment. Results: Among AECOPD patients, there were 22 infrequent and 55 frequent exacerbators. Infrequent exacerbators showed better muscle parameters, extracellular water ratio, phase angle, and handgrip strength. Significant differences in intracellular water, total cellular water, protein, and body cell mass were observed between groups. Logistic regression indicated that extracellular water ratio (OR = 1.086) and phase angle (OR = 0.396) were independently associated with exacerbation risk. Thresholds for exacerbation risk were identified as 0.393 for extracellular water ratio and 4.85° for phase angle. In stable COPD, 13 frequent and 69 infrequent exacerbators were compared, showing no significant differences in weight, muscle, and adipose parameters, but significant differences in extracellular water ratio, phase angle, and handgrip strength. Conclusions: These findings suggest that increased exacerbations in COPD patients correlate with higher extracellular water ratios and lower phase angles.
Full article
Open AccessArticle
Cross-Reactivity of Ragweed Pollen Calcium-Binding Proteins and IgE Sensitization in a Ragweed-Allergic Population from Western Romania
by
Lauriana-Eunice Zbîrcea, Maria-Roxana Buzan, Manuela Grijincu, Tudor-Paul Tamaș, Constantina Bianca Vulpe, Ioan Huțu, Virgil Păunescu, Carmen Panaitescu and Kuan-Wei Chen
Adv. Respir. Med. 2024, 92(3), 218-229; https://doi.org/10.3390/arm92030022 (registering DOI) - 30 May 2024
Abstract
Ragweed pollen allergy is the most common seasonal allergy in western Romania. Prolonged exposure to ragweed pollen may induce sensitization to pan-allergens such as calcium-binding proteins (polcalcins) and progression to more severe symptoms. We aimed to detect IgE sensitization to recombinant Amb a
[...] Read more.
Ragweed pollen allergy is the most common seasonal allergy in western Romania. Prolonged exposure to ragweed pollen may induce sensitization to pan-allergens such as calcium-binding proteins (polcalcins) and progression to more severe symptoms. We aimed to detect IgE sensitization to recombinant Amb a 9 and Amb a 10 in a Romanian population, to assess their potential clinical relevance and cross-reactivity, as well as to investigate the relation with clinical symptoms. rAmb a 9 and rAmb a 10 produced in Escherichia coli were used to detect specific IgE in sera from 87 clinically characterized ragweed-allergic patients in ELISA, for basophil activation experiments and rabbit immunization. Rabbit rAmb a 9- and rAmb a 10-specific sera were used to detect possible cross-reactivity with rArt v 5 and reactivity towards ragweed and mugwort pollen extracts. The results showed an IgE reactivity of 25% to rAmb a 9 and 35% to rAmb a 10. rAmb a 10 induced basophil degranulation in three out of four patients tested. Moreover, polcalcin-negative patients reported significantly more skin symptoms, whereas polcalcin-positive patients tended to report more respiratory symptoms. Furthermore, both rabbit antisera showed low reactivity towards extracts and showed high reactivity to rArt v 5, suggesting strong cross-reactivity. Our study indicated that recombinant ragweed polcalcins might be considered for molecular diagnosis.
Full article
Open AccessArticle
RNA Polymerase Inhibitor Enisamium for Treatment of Moderate COVID-19 Patients: A Randomized, Placebo-Controlled, Multicenter, Double-Blind Phase 3 Clinical Trial
by
Olga Holubovska, Pavlo Babich, Alla Mironenko, Jens Milde, Yuriy Lebed, Holger Stammer, Lutz Mueller, Aartjan J. W. te Velthuis, Victor Margitich and Andrew Goy
Adv. Respir. Med. 2024, 92(3), 202-217; https://doi.org/10.3390/arm92030021 - 6 May 2024
Abstract
►▼
Show Figures
Enisamium is an orally available therapeutic that inhibits influenza A virus and SARS-CoV-2 replication. We evaluated the clinical efficacy of enisamium treatment combined with standard care in adult, hospitalized patients with moderate COVID-19 requiring external oxygen. Hospitalized patients with laboratory-confirmed SARS-CoV-2 infection were
[...] Read more.
Enisamium is an orally available therapeutic that inhibits influenza A virus and SARS-CoV-2 replication. We evaluated the clinical efficacy of enisamium treatment combined with standard care in adult, hospitalized patients with moderate COVID-19 requiring external oxygen. Hospitalized patients with laboratory-confirmed SARS-CoV-2 infection were randomly assigned to receive either enisamium (500 mg per dose, four times a day) or a placebo. The primary outcome was an improvement of at least two points on an eight-point severity rating (SR) scale within 29 days of randomization. We initially set out to study the effect of enisamium on patients with a baseline SR of 4 or 5. However, because the study was started early in the COVID-19 pandemic, and COVID-19 had been insufficiently studied at the start of our study, an interim analysis was performed alongside a conditional power analysis in order to ensure patient safety and assess whether the treatment was likely to be beneficial for one or both groups. Following this analysis, a beneficial effect was observed for patients with an SR of 4 only, i.e., patients with moderate COVID-19 requiring supplementary oxygen. The study was continued for these COVID-19 patients. Overall, a total of 592 patients were enrolled and randomized between May 2020 and March 2021. Patients with a baseline SR of 4 were divided into two groups: 142 (49.8%) were assigned to the enisamium group and 143 (50.2%) to the placebo group. An analysis of the population showed that if patients were treated within 4 days of the onset of COVID-19 symptoms (n = 33), the median time to improvement was 8 days for the enisamium group and 13 days for the placebo group (p = 0.005). For patients treated within 10 days of the onset of COVID-19 symptoms (n = 154), the median time to improvement was 10 days for the enisamium group and 12 days for the placebo group (p = 0.002). Our findings suggest that enisamium is safe to use with COVID-19 patients, and that the observed clinical benefit of enisamium is worth reporting and studying in detail.
Full article

Figure 1
Open AccessReview
Diagnostic Value of Imaging and Serological Biomarkers in Pulmonary Sarcoidosis
by
Yuehong Li and Guopeng Xu
Adv. Respir. Med. 2024, 92(3), 190-201; https://doi.org/10.3390/arm92030020 - 28 Apr 2024
Abstract
►▼
Show Figures
Sarcoidosis is a multisystem granulomatous disease of an unknown aetiology. It can exist in many organs. Pulmonary and intrathoracic lymph nodes are most commonly involved. Lung sarcoidosis is uncommon in Asia. However, due to the large population of our country and the development
[...] Read more.
Sarcoidosis is a multisystem granulomatous disease of an unknown aetiology. It can exist in many organs. Pulmonary and intrathoracic lymph nodes are most commonly involved. Lung sarcoidosis is uncommon in Asia. However, due to the large population of our country and the development of bronchoscopy, percutaneous lung puncture, and other medical technologies, the number of pulmonary sarcoidosis patients is on the rise. Pulmonary sarcoidosis patients have no obvious symptoms in the early stage, and the clinical manifestations in the later stage may vary from person to person. Eventually, the disease progresses to life-threatening pulmonary fibrosis. Therefore, patients with pulmonary sarcoidosis should receive a timely diagnosis. In recent years, the imaging features and serologic biomarkers of pulmonary sarcoidosis have been continuously studied. The diagnostic value of imaging and serologic biomarkers for pulmonary sarcoidosis is summarized below.
Full article
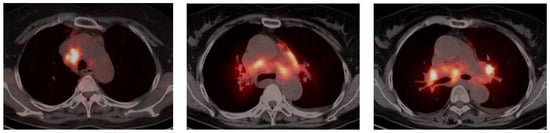
Figure 1
Open AccessSystematic Review
Nurses’ Role in the Control and Treatment of Asthma in Adults: A Systematic Literature Review
by
Pedro Alexandre-Sousa, Nuno Sousa, Joana Bento, Filipa Azevedo, Maíra Assis and José Mendes
Adv. Respir. Med. 2024, 92(3), 175-189; https://doi.org/10.3390/arm92030019 - 25 Apr 2024
Abstract
►▼
Show Figures
Bronchial asthma is a chronic pathology and a global public health problem. However, asthma can be controlled and treated for the most part by patients, so the Portuguese General Directorate of Health recommends shared medical appointments in primary health care (PHC). The present
[...] Read more.
Bronchial asthma is a chronic pathology and a global public health problem. However, asthma can be controlled and treated for the most part by patients, so the Portuguese General Directorate of Health recommends shared medical appointments in primary health care (PHC). The present study aims to identify the role of PHC nurses in the control and treatment of asthma in adults. Using the MeSH platform, the following descriptors were validated: asthma, nurses, adults. An individual search was carried out in the following databases: CINAHL (ESBSCO host), MEDLINE (Pubmed host), Web of Science, and Scopus. Out of a total of 280 publications, 79 of which were duplicates and 185 publications which did not meet the inclusion criteria, 16 publications remained readable. Of the eligible articles, there were 13 specialist reports, one mixed study, one quasi-experimental study, and one randomized trial. Education was the intervention most identified in the scientific evidence analyzed, and patient assessment, application of an asthma control questionnaire, verification and training of inhalation technique, empowerment for self-management of the disease, support, promotion of seasonal influenza vaccination, and use of written action plans were also identified. The results reveal that, although the scientific evidence on the intervention of these professionals is poorly developed, nurses play a crucial role in the control and treatment of asthma. The scientific evidence analyzed allowed the identification of interventions that can help the organization of a nursing health appointment, providing nurses with a crucial role in the control and treatment of asthma in adults in the context of PHC.
Full article
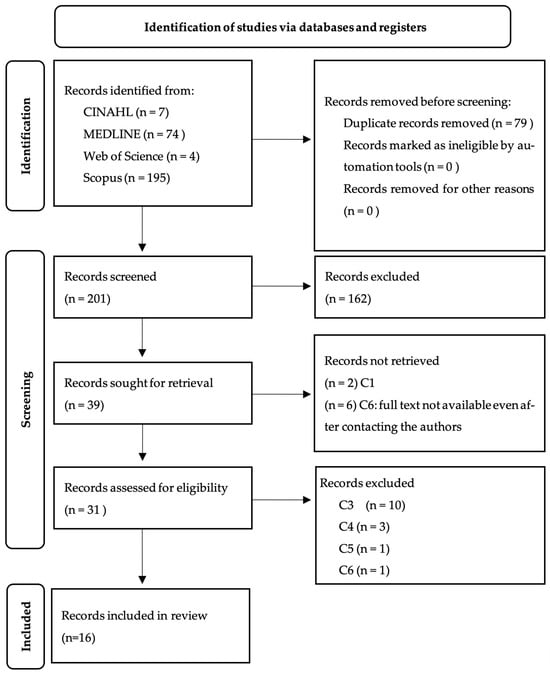
Figure 1
Open AccessSystematic Review
How to Enhance the Diagnosis of Early Stages of Chronic Obstructive Pulmonary Disease (COPD)? The Role of Mobile Spirometry in COPD Screening and Diagnosis—A Systematic Review
by
Piotr Jankowski, Katarzyna Mycroft, Katarzyna Górska, Piotr Korczyński and Rafał Krenke
Adv. Respir. Med. 2024, 92(2), 158-174; https://doi.org/10.3390/arm92020018 - 27 Mar 2024
Abstract
►▼
Show Figures
COPD is the third leading cause of death worldwide. Its diagnosis can be made with spirometry, which is underused due to its limited accessibility. Portable spirometry holds promise for enhancing the efficacy of COPD diagnoses. The study aimed to estimate COPD prevalence diagnosed
[...] Read more.
COPD is the third leading cause of death worldwide. Its diagnosis can be made with spirometry, which is underused due to its limited accessibility. Portable spirometry holds promise for enhancing the efficacy of COPD diagnoses. The study aimed to estimate COPD prevalence diagnosed with a portable spirometer in high-risk patients and compare it with COPD prevalence based on data from conventional, on-site spirometry. We also evaluated the strategy of a proactive approach to identify COPD in high-risk individuals. We conducted a systematic review of original studies on COPD targeted screening and diagnosis with portable and conventional spirometers selected from 8496 publications initially found in three databases: Cochrane, PubMed, and Embase. The inclusion criteria were met by 28 studies. COPD prevalence evaluated with the use of portable spirometers reached 20.27% and was lower compared to that estimated with the use of conventional spirometers (24.67%). In 11 included studies, postbronchodilator tests were performed with portable spirometers, which enabled a bedside COPD diagnosis. Portable spirometers can be successfully used in COPD targeted screening and diagnosis and thus enhance the detection of COPD at early stages.
Full article
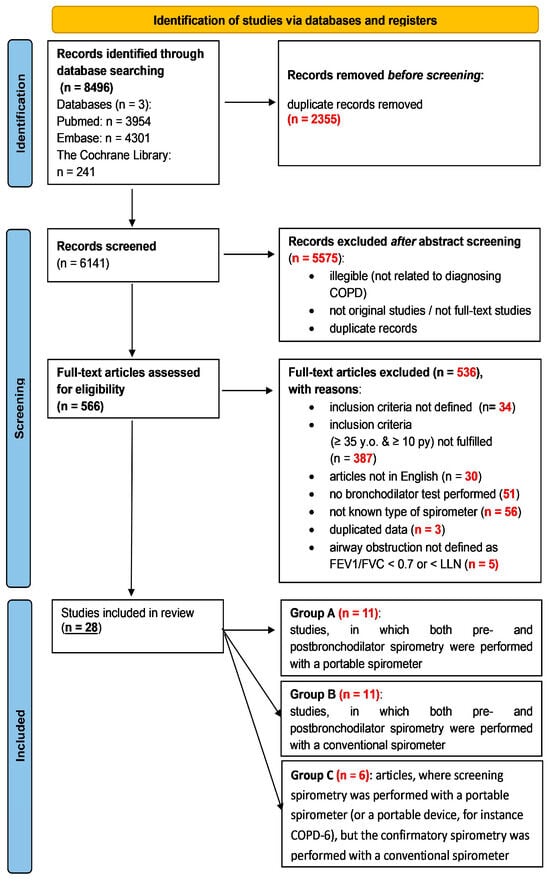
Figure 1
Open AccessEditorial
Advances in Respiratory Medicine—Aims and Scopes Update
by
Krzysztof Kuziemski, Monika Franczuk, Sebastian Majewski, Tadeusz M. Zielonka and Adam Barczyk
Adv. Respir. Med. 2024, 92(2), 156-157; https://doi.org/10.3390/arm92020017 - 19 Mar 2024
Abstract
Advances in Respiratory Medicine, which has been published by MDPI since 2022, serves as a platform for hosting pneumological studies [...]
Full article
Open AccessArticle
Outcomes and Functional Deterioration in Hospital Admissions with Acute Hypoxemia
by
Susanne Simon, Jens Gottlieb, Ina Burchert, René Abu Isneineh and Thomas Fuehner
Adv. Respir. Med. 2024, 92(2), 145-155; https://doi.org/10.3390/arm92020016 - 6 Mar 2024
Abstract
►▼
Show Figures
Background: Many hospitalized patients decline in functional status after discharge, but functional decline in emergency admissions with hypoxemia is unknown. The primary aim of this study was to study functional outcomes as a clinical endpoint in a cohort of patients with acute hypoxemia.
[...] Read more.
Background: Many hospitalized patients decline in functional status after discharge, but functional decline in emergency admissions with hypoxemia is unknown. The primary aim of this study was to study functional outcomes as a clinical endpoint in a cohort of patients with acute hypoxemia. Methods: A multicenter prospective observational study was conducted in patients with new-onset hypoxemia emergently admitted to two respiratory departments at a university hospital and an academic teaching hospital. Using the WHO scale, the patients’ functional status 4 weeks before admission and at hospital discharge was assessed. The type and duration of oxygen therapy, hospital length of stay and survival and risk of hypercapnic failure were recorded. Results: A total of 151 patients with a median age of 74 were included. Two-thirds declined in functional status by at least one grade at discharge. A good functional status (OR 4.849 (95% CI 2.209–10.647)) and progressive cancer (OR 6.079 (1.197–30.881)) were more associated with functional decline. Most patients were treated with conventional oxygen therapy (n = 95, 62%). The rates of in-hospital mortality and need for intubation were both 8%. Conclusions: Patients with acute hypoxemia in the emergency room have a poorer functional status after hospital discharge. This decline may be of multifactorial origin.
Full article
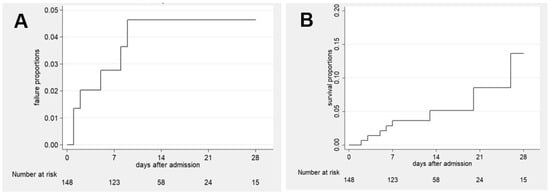
Figure 1
Open AccessArticle
Association between the Static and Dynamic Lung Function and CT-Derived Thoracic Skeletal Muscle Measurements–A Retrospective Analysis of a 12-Month Observational Follow-Up Pilot Study
by
Mia Solholt Godthaab Brath, Sisse Dyrman Alsted, Marina Sahakyan, Esben Bolvig Mark, Jens Brøndum Frøkjær, Henrik Højgaard Rasmussen, Lasse Riis Østergaard, Rasmus Brath Christensen and Ulla Møller Weinreich
Adv. Respir. Med. 2024, 92(2), 123-144; https://doi.org/10.3390/arm92020015 - 6 Mar 2024
Abstract
►▼
Show Figures
Background: Patients with chronic obstructive pulmonary disease (COPD) with low skeletal muscle mass and severe airway obstruction have higher mortality risks. However, the relationship between dynamic/static lung function (LF) and thoracic skeletal muscle measurements (SMM) remains unclear. This study explored patient characteristics (weight,
[...] Read more.
Background: Patients with chronic obstructive pulmonary disease (COPD) with low skeletal muscle mass and severe airway obstruction have higher mortality risks. However, the relationship between dynamic/static lung function (LF) and thoracic skeletal muscle measurements (SMM) remains unclear. This study explored patient characteristics (weight, BMI, exacerbations, dynamic/static LF, sex differences in LF and SMM, and the link between LF and SMM changes. Methods: A retrospective analysis of a 12-month prospective follow-up study patients with stable COPD undergoing standardized treatment, covering mild to severe stages, was conducted. The baseline and follow-up assessments included computed tomography and body plethysmography. Results: This study included 35 patients (17 females and 18 males). This study revealed that females had more stable LF but tended to have greater declines in SMM areas and indices than males (−5.4% vs. −1.9%, respectively), despite the fact that females were younger and had higher LF and less exacerbation than males. A multivariate linear regression showed a negative association between the inspiratory capacity/total lung capacity ratio (IC/TLC) and muscle fat area. Conclusions: The findings suggest distinct LF and BC progression patterns between male and female patients with COPD. A low IC/TLC ratio may predict increased muscle fat. Further studies are necessary to understand these relationships better.
Full article
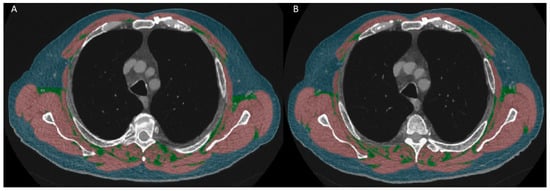
Figure 1
Open AccessReview
Advancing Care in Severe Asthma: The Art of Switching Biologics
by
Silvano Dragonieri, Andrea Portacci, Vitaliano Nicola Quaranta and Giovanna Elisiana Carpagnano
Adv. Respir. Med. 2024, 92(2), 110-122; https://doi.org/10.3390/arm92020014 - 21 Feb 2024
Abstract
►▼
Show Figures
Biologics targeting IgE, IL-5, IL-4/IL-13, and TSLP are crucial in severe asthma treatment. Research, including randomized controlled trials and real-world studies, has been conducted to assess their efficacy and identify patient characteristics that may predict positive responses. The effectiveness of switching biologics, especially
[...] Read more.
Biologics targeting IgE, IL-5, IL-4/IL-13, and TSLP are crucial in severe asthma treatment. Research, including randomized controlled trials and real-world studies, has been conducted to assess their efficacy and identify patient characteristics that may predict positive responses. The effectiveness of switching biologics, especially given overlaps in treatment eligibility, and the clinical outcomes post-cessation are critical areas of investigation. This work reviews the effects of switching between these biologics and the indicators of treatment success or failure. Insights are primarily derived from real-world experiences, focusing on patients transitioning from one monoclonal antibody to another. Moreover, this review aims to provide insights into the effectiveness, safety, and broader implications of switching biologics, enhancing understanding for clinicians to optimize severe asthma management. The article underlines the importance of a patient-centered approach, biomarker assessment, and the evolving nature of asthma treatment in making informed decisions about biologic therapy.
Full article
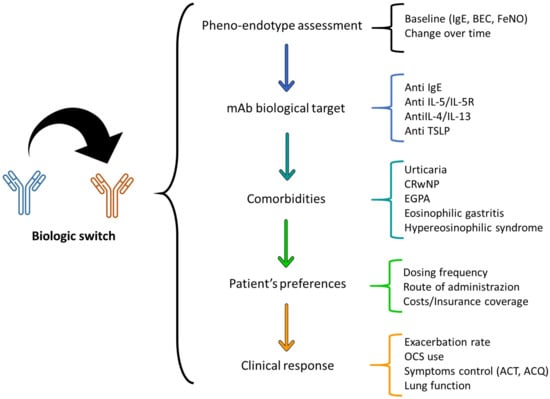
Figure 1
Open AccessReview
The Growing Understanding of the Pituitary Implication in the Pathogenesis of Long COVID-19 Syndrome: A Narrative Review
by
Ach Taieb, Ben Haj Slama Nassim, Gorchane Asma, Methnani Jabeur, Saad Ghada and Ben Abdelkrim Asma
Adv. Respir. Med. 2024, 92(1), 96-109; https://doi.org/10.3390/arm92010013 - 14 Feb 2024
Cited by 1
Abstract
Long COVID-19, also known as post-acute sequelae of SARS-CoV-2 infection, is a condition where individuals who have recovered from the acute phase of COVID-19 continue to experience a range of symptoms for weeks or even months afterward. While it was initially thought to
[...] Read more.
Long COVID-19, also known as post-acute sequelae of SARS-CoV-2 infection, is a condition where individuals who have recovered from the acute phase of COVID-19 continue to experience a range of symptoms for weeks or even months afterward. While it was initially thought to primarily affect the respiratory system, it has become clear that Long COVID-19 can involve various organs and systems, including the endocrine system, which includes the pituitary gland. In the context of Long COVID-19, there is a growing understanding of the potential implications for the pituitary gland. The virus can directly affect the pituitary gland, leading to abnormalities in hormone production and regulation. This can result in symptoms such as fatigue, changes in appetite, and mood disturbances. Long COVID-19, the persistent and often debilitating condition following acute COVID-19 infection, may be explained by deficiencies in ACTH and Growth hormone production from the pituitary gland. Corticotropin insufficiency can result in the dysregulation of the body’s stress response and can lead to prolonged feelings of stress, fatigue, and mood disturbances in Long COVID-19 patients. Simultaneously, somatotropin insufficiency can affect growth, muscle function, and energy metabolism, potentially causing symptoms such as muscle weakness, exercise intolerance, and changes in body composition. Recently, some authors have suggested the involvement of the pituitary gland in Post COVID-19 Syndrome. The exact mechanisms of viral action on infected cells remain under discussion, but inflammatory and autoimmune mechanisms are primarily implicated. The aim of our study will be to review the main pituitary complications following COVID-19 infection. Moreover, we will explain the possible involvement of the pituitary gland in the persistence of Post COVID-19 Syndrome.
Full article
Open AccessCommentary
Administering Nitric Oxide (NO) with High Flow Nasal Cannulas: A Simple Method
by
Vladimir L. Cousin, Raphael Joye and Angelo Polito
Adv. Respir. Med. 2024, 92(1), 92-95; https://doi.org/10.3390/arm92010012 - 8 Feb 2024
Cited by 1
Abstract
►▼
Show Figures
Inhaled nitric oxide (iNO) is a pulmonary vasodilator that plays an important clinical ICU role. The administration of iNO is usually performed through an endotracheal tube, but spontaneously breathing patients might also benefit from iNO administration. The use of the non-invasive administration of
[...] Read more.
Inhaled nitric oxide (iNO) is a pulmonary vasodilator that plays an important clinical ICU role. The administration of iNO is usually performed through an endotracheal tube, but spontaneously breathing patients might also benefit from iNO administration. The use of the non-invasive administration of iNO through high-flow nasal cannula (HFNC) allows for NO delivery in spontaneously breathing patients who still need supplemental oxygen and positive airway pressure. A simple method to administer NO through HFNC is described here using standard commercially available NO administration and HFNC.
Full article
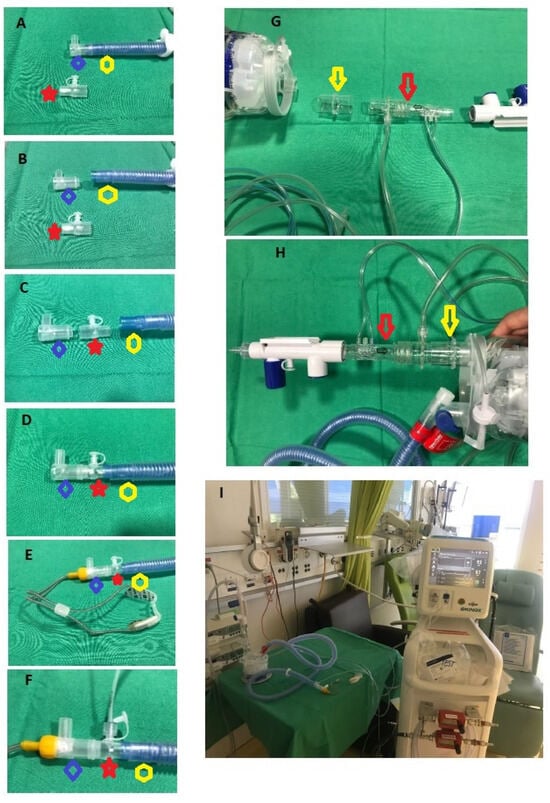
Figure 1
Open AccessCorrection
Correction: Patsaki et al. Benefits from Incorporating Virtual Reality in Pulmonary Rehabilitation of COPD Patients: A Systematic Review and Meta-Analysis. Adv. Respir. Med. 2023, 91, 324–336
by
Irini Patsaki, Vasiliki Avgeri, Theodora Rigoulia, Theodoros Zekis, George A. Koumantakis and Eirini Grammatopoulou
Adv. Respir. Med. 2024, 92(1), 89-91; https://doi.org/10.3390/arm92010011 - 1 Feb 2024
Abstract
►▼
Show Figures
Error in Figure 3 [...]
Full article
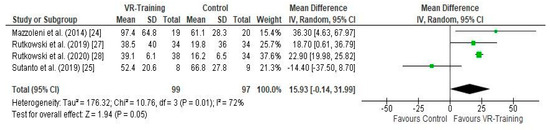
Figure 3
Open AccessArticle
Constructing a Nomogram Model to Estimate the Risk of Ventilator-Associated Pneumonia for Elderly Patients in the Intensive Care Unit
by
Wensi Gan, Zhihui Chen, Zhen Tao and Wenyuan Li
Adv. Respir. Med. 2024, 92(1), 77-88; https://doi.org/10.3390/arm92010010 - 19 Jan 2024
Abstract
►▼
Show Figures
Background: Ventilator-associated pneumonia (VAP) causes heavy losses in terms of finances, hospitalization, and death for elderly patients in the intensive care unit (ICU); however, the risk is difficult to evaluate due to a lack of reliable assessment tools. We aimed to create and
[...] Read more.
Background: Ventilator-associated pneumonia (VAP) causes heavy losses in terms of finances, hospitalization, and death for elderly patients in the intensive care unit (ICU); however, the risk is difficult to evaluate due to a lack of reliable assessment tools. We aimed to create and validate a nomogram to estimate VAP risk to provide early intervention for high-risk patients. Methods: Between January 2016 and March 2021, 293 patients from a tertiary hospital in China were retrospectively reviewed as a training set. Another 84 patients were enrolled for model validation from April 2021 to February 2022. Least absolute shrinkage and selection operator (LASSO) regression and multivariable logistic regression analysis were employed to select predictors, and a nomogram model was constructed. The calibration, discrimination, and clinical utility of the nomogram were verified. Finally, a web-based online scoring system was created to make the model more practical. Results: The predictors were hypoproteinemia, long-term combined antibiotic use, intubation time, length of mechanical ventilation, and tracheotomy/intubation. The area under the curve (AUC) was 0.937 and 0.925 in the training and validation dataset, respectively, suggesting the model exhibited effective discrimination. The calibration curve demonstrated high consistency with the observed result and the estimated values. Decision curve analysis (DCA) demonstrated that the nomogram was clinically applicable. Conclusions: We have created a novel nomogram model that can be utilized to anticipate VAP risk in elderly ICU patients, which is helpful for healthcare professionals to detect patients at high risk early and adopt protective interventions.
Full article
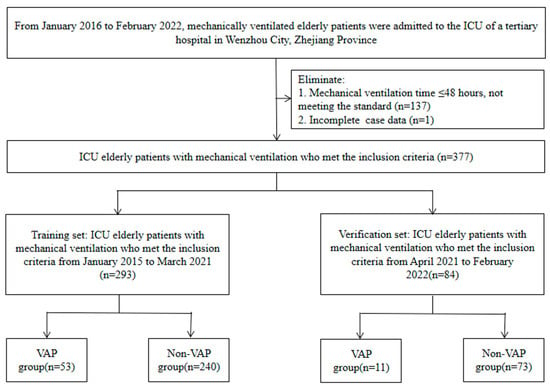
Figure 1
Open AccessReview
Clinical Effectiveness of Ritonavir-Boosted Nirmatrelvir—A Literature Review
by
Sydney Paltra and Tim O. F. Conrad
Adv. Respir. Med. 2024, 92(1), 66-76; https://doi.org/10.3390/arm92010009 - 18 Jan 2024
Abstract
Nirmatrelvir/Ritonavir is an oral treatment for mild to moderate COVID-19 cases with a high risk for a severe course of the disease. For this paper, a comprehensive literature review was performed, leading to a summary of currently available data on Nirmatrelvir/Ritonavir’s ability to
[...] Read more.
Nirmatrelvir/Ritonavir is an oral treatment for mild to moderate COVID-19 cases with a high risk for a severe course of the disease. For this paper, a comprehensive literature review was performed, leading to a summary of currently available data on Nirmatrelvir/Ritonavir’s ability to reduce the risk of progressing to a severe disease state. Herein, the focus lies on publications that include comparisons between patients receiving Nirmatrelvir/Ritonavir and a control group. The findings can be summarized as follows: Data from the time when the Delta-variant was dominant show that Nirmatrelvir/Ritonavir reduced the risk of hospitalization or death by 88.9% for unvaccinated, non-hospitalized high-risk individuals. Data from the time when the Omicron variant was dominant found decreased relative risk reductions for various vaccination statuses: between 26% and 65% for hospitalization. The presented papers that differentiate between unvaccinated and vaccinated individuals agree that unvaccinated patients benefit more from treatment with Nirmatrelvir/Ritonavir. However, when it comes to the dependency of potential on age and comorbidities, further studies are necessary. From the available data, one can conclude that Nirmatrelvir/Ritonavir cannot substitute vaccinations; however, its low manufacturing cost and easy administration make it a valuable tool in fighting COVID-19, especially for countries with low vaccination rates.
Full article
Open AccessArticle
Breathing Pattern Response after 6 Weeks of Inspiratory Muscle Training during Exercise
by
Eduardo Salazar-Martínez
Adv. Respir. Med. 2024, 92(1), 58-65; https://doi.org/10.3390/arm92010008 - 17 Jan 2024
Abstract
►▼
Show Figures
(1) Background: The breathing pattern is defined as the relationship between the tidal volume (VT) and breathing frequency (BF) for a given VE. The aim of this study was to evaluate whether inspiratory muscle training influenced the response of the breathing pattern during
[...] Read more.
(1) Background: The breathing pattern is defined as the relationship between the tidal volume (VT) and breathing frequency (BF) for a given VE. The aim of this study was to evaluate whether inspiratory muscle training influenced the response of the breathing pattern during an incremental effort in amateur cyclists. (2) Methods: Eighteen amateur cyclists completed an incremental test to exhaustion, and a gas analysis on a cycle ergometer and spirometry were conducted. Cyclists were randomly assigned to two groups (IMTG = 9; CON = 9). The IMTG completed 6 weeks of inspiratory muscle training (IMT) using a PowerBreathe K3® device at 50% of the maximum inspiratory pressure (Pimax). The workload was adjusted weekly. The CON did not carry out any inspiratory training during the experimental period. After the 6-week intervention, the cyclists repeated the incremental exercise test, and the gas analysis and spirometry were conducted. The response of the breathing pattern was evaluated during the incremental exercise test. (3) Results: The Pimax increased in the IMTG (p < 0.05; d = 3.1; +19.62%). Variables related to the breathing pattern response showed no differences between groups after the intervention (EXPvsCON; p > 0.05). Likewise, no differences in breathing pattern were found in the IMTG after training (PREvsPOST; p > 0.05). (4) Conclusions: IMT improved the strength of inspiratory muscles and sport performance in amateur cyclists. These changes were not attributed to alterations in the response of the breathing pattern.
Full article
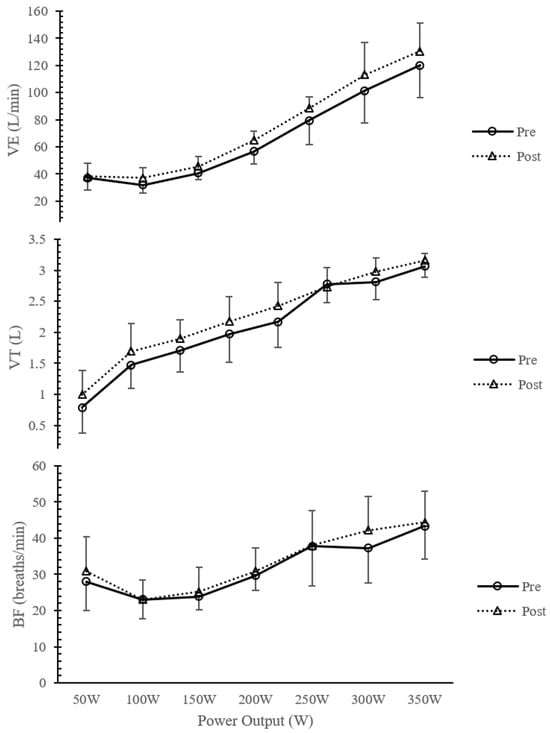
Figure 1
Open AccessArticle
Pulmonary Embolism (PE) to Chronic Thromboembolic Pulmonary Disease (CTEPD): Findings from a Survey of UK Physicians
by
Joanna Pepke-Zaba, Luke Howard, David G. Kiely, Shruti Sweeney and Martin Johnson
Adv. Respir. Med. 2024, 92(1), 45-57; https://doi.org/10.3390/arm92010007 - 9 Jan 2024
Abstract
►▼
Show Figures
Chronic thromboembolic pulmonary disease (CTEPD) is a complication of pulmonary embolism (PE). We conducted an online survey of UK PE-treating physicians to understand practices in the follow-up of PE and awareness of CTEPD. The physicians surveyed (N = 175) included 50 each
[...] Read more.
Chronic thromboembolic pulmonary disease (CTEPD) is a complication of pulmonary embolism (PE). We conducted an online survey of UK PE-treating physicians to understand practices in the follow-up of PE and awareness of CTEPD. The physicians surveyed (N = 175) included 50 each from cardiology, respiratory and internal medicine, plus 25 haematologists. Most (89%) participants had local guidelines for PE management, and 65% reported a PE follow-up clinic, of which 69% were joint clinics. Almost half (47%) had a protocol for the investigation of CTEPD. According to participants, 129 (74%) routinely consider a diagnosis of CTEPD and 97 (55%) routinely investigate for CTEPD, with 76% of those 97 participants investigating in patients who are symptomatic at 3 months and 22% investigating in all patients. This survey demonstrated variability in the follow-up of PE and the awareness of CTEPD and its investigation. The findings support the conduct of a national audit to understand the barriers to the timely detection of CTEPD.
Full article
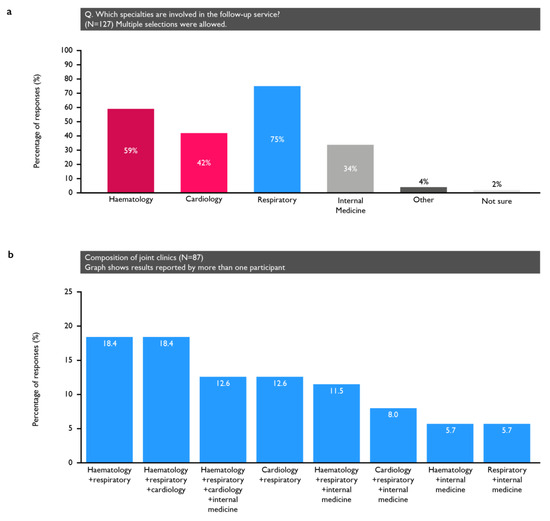
Figure 1
Open AccessArticle
Predictive Value of Fractional Exhaled Nitric Oxide (FeNO) in the Diagnosis of Asthma for Epidemiological Purposes—An 8-Year Follow-Up Study
by
Kamil Barański
Adv. Respir. Med. 2024, 92(1), 36-44; https://doi.org/10.3390/arm92010006 - 4 Jan 2024
Abstract
At the population level, respiratory symptoms in children can be estimated cross-sectionally. However, such methods require additional objective support parameters, such as the measurement of fractional exhaled nitric oxide (FeNO). The aim of the present study was to analyze if the FeNO value
[...] Read more.
At the population level, respiratory symptoms in children can be estimated cross-sectionally. However, such methods require additional objective support parameters, such as the measurement of fractional exhaled nitric oxide (FeNO). The aim of the present study was to analyze if the FeNO value measured at baseline can have a predictive value for asthma-like symptoms after 8 years of measurement. Methods: The follow-up included 128 (out of 447) children, 70 girls and 58 boys. The FeNO was measured at baseline only. The prevalence of asthma-like symptoms was measured with the adopted version of the ISAAC questionnaire. Results: After 8 years of FeNO measurement, 5 new cases of asthma, 2 cases of attacks of dyspnoea, 1 case of wheezy in the chest, and 18 cases of allergic rhinitis occurred. The FeNO values, measured at the baseline of the study, for new cases of the above diseases were 53.4 ± 75.9 ppb, 11 ± 1.5 ppb, 12.0 ppb, and 16.3 ± 12.4 ppb, respectively. The best diagnostic accuracy parameters were found in the new cases of asthma, where the sensitivity was 40.0%, the specificity was 98.6%, and the AUC was 66.6%. The diagnostic odds ratio was 46.9 when considering the FeNO cut-off >35 ppb. Conclusions: The FeNO measurement is a fair method for asthma prognosis in early school-aged children with asthma-like symptoms measured on the population level but requires further confirmation at the clinical level with more accurate diagnostic tools.
Full article
Open AccessBrief Report
Expression of Inflammatory Genes in Murine Lungs in a Model of Experimental Pulmonary Hypertension: Effects of an Antibody-Based Targeted Delivery of Interleukin-9
by
Judith Heiss, Katja Grün, Isabell Singerer, Laura Tempel, Mattia Matasci, Christian Jung, Alexander Pfeil, P. Christian Schulze, Dario Neri and Marcus Franz
Adv. Respir. Med. 2024, 92(1), 27-35; https://doi.org/10.3390/arm92010005 - 3 Jan 2024
Abstract
►▼
Show Figures
Background: Pathogenesis of pulmonary hypertension (PH) is a multifactorial process driven by inflammation and pulmonary vascular remodeling. To target these two aspects of PH, we recently tested a novel treatment: Interleukin-9 (IL9) fused to F8, an antibody that binds to the extra-domain A
[...] Read more.
Background: Pathogenesis of pulmonary hypertension (PH) is a multifactorial process driven by inflammation and pulmonary vascular remodeling. To target these two aspects of PH, we recently tested a novel treatment: Interleukin-9 (IL9) fused to F8, an antibody that binds to the extra-domain A of fibronectin (EDA+ Fn). As EDA+ Fn is not found in healthy adult tissue but is expressed during PH, IL9 is delivered specifically to the tissue affected by PH. We found that F8IL9 reduced pulmonary vascular remodeling and attenuated PH compared with sham-treated mice. Purpose: To evaluate possible F8IL9 effects on PH-associated inflammatory processes, we analysed the expression of genes involved in pulmonary immune responses. Methods: We applied the monocrotaline (MCT) model of PH in mice (n = 44). Animals were divided into five experimental groups: sham-induced animals without PH (control, n = 4), MCT-induced PH without treatment (PH, n = 8), dual endothelin receptor antagonist treatment (dual ERA, n = 8), F8IL9 treatment (n = 12, 2 formats with n = 6 each), or with KSFIL9 treatment (KSFIL9, n = 12, 2 formats with n = 6 each, KSF: control antibody with irrelevant antigen specificity). After 28 days, a RT-PCR gene expression analysis of inflammatory response (84 genes) was performed in the lung. Results: Compared with the controls, 19 genes exhibited relevant (+2.5-fold) upregulation in the PH group without treatment. Gene expression levels in F8IL9-treated lung tissue were reduced compared to the PH group without treatment. This was the case especially for CCL20, CXCL5, C-reactive protein, pentraxin related (CRPPR), and Kininogen-1 (KNG1). Conclusion: In accordance with the hypothesis stated above, F8IL9 treatment diminished the upregulation of some genes associated with inflammation in a PH animal model. Therefore, we hypothesize that IL9-based immunocytokine treatment will likely modulate various inflammatory pathways.
Full article
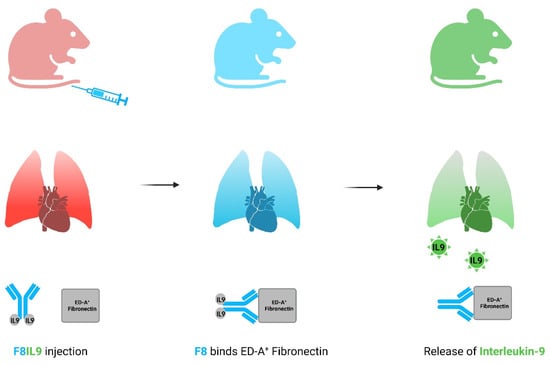
Figure 1
Open AccessReply
Reply to Salimi, M. Comment on “Patsaki et al. Benefits from Incorporating Virtual Reality in Pulmonary Rehabilitation of COPD Patients: A Systematic Review and Meta-Analysis. Adv. Respir. Med. 2023, 91, 324–336”
by
Irini Patsaki, Vasiliki Avgeri, Theodora Rigoulia, Theodoros Zekis, George A. Koumantakis and Eirini Grammatopoulou
Adv. Respir. Med. 2024, 92(1), 25-26; https://doi.org/10.3390/arm92010004 - 22 Dec 2023
Abstract
We are writing in response to the comment [...]
Full article

Journal Menu
► ▼ Journal MenuJournal Browser
► ▼ Journal Browser-
arrow_forward_ios
Forthcoming issue
arrow_forward_ios Current issue - Volumes not published by MDPI
Highly Accessed Articles
Latest Books
E-Mail Alert
News
Topics
Topic in
JCDD, JCM, Medicina, Membranes, ARM
Extracorporeal Membrane Oxygenation (ECMO)
Topic Editors: Patrick Honore, Isabelle MichauxDeadline: 30 November 2024

Conferences
Special Issues
Special Issue in
ARM
Respiratory Rehabilitation: Current Perspectives and Future Challenges
Guest Editors: Luís Sousa, Helena José, Isabel RabiaisDeadline: 12 July 2024
Special Issue in
ARM
Expanding Usage of Non-invasive Positive Pressure Ventilation
Guest Editor: Mandeep Singh RahiDeadline: 6 December 2024





