-
 The Relationship between Fine Particle Matter (PM2.5) Exposure and Upper Respiratory Tract Diseases
The Relationship between Fine Particle Matter (PM2.5) Exposure and Upper Respiratory Tract Diseases -
 Adult Congenital Heart Disease in the Emergency Department
Adult Congenital Heart Disease in the Emergency Department -
 Low CDKN1B Expression Associated with Reduced CD8+ T Lymphocytes Predicts Poor Outcome in Breast Cancer in a Machine Learning Analysis
Low CDKN1B Expression Associated with Reduced CD8+ T Lymphocytes Predicts Poor Outcome in Breast Cancer in a Machine Learning Analysis -
 Sepsis Stewardship: The Puzzle of the Antibiotic Therapy in the Context of Individualization of Decision Making
Sepsis Stewardship: The Puzzle of the Antibiotic Therapy in the Context of Individualization of Decision Making -
 Inhibitors of Immune Checkpoints: Small Molecule- and Peptide-Based Approaches
Inhibitors of Immune Checkpoints: Small Molecule- and Peptide-Based Approaches
Journal Description
Journal of Personalized Medicine
Journal of Personalized Medicine
is an international, peer-reviewed, open access journal on personalized medicine, published monthly online by MDPI.
- Open Access— free for readers, with article processing charges (APC) paid by authors or their institutions.
- High Visibility: indexed within Scopus, SCIE (Web of Science), PubMed, PMC, Embase, and other databases.
- Journal Rank: JCR - Q2 (Medicine, General & Internal) CiteScore - Q2 (Medicine (miscellaneous))
- Rapid Publication: manuscripts are peer-reviewed and a first decision is provided to authors approximately 17.8 days after submission; acceptance to publication is undertaken in 2.6 days (median values for papers published in this journal in the second half of 2023).
- Recognition of Reviewers: reviewers who provide timely, thorough peer-review reports receive vouchers entitling them to a discount on the APC of their next publication in any MDPI journal, in appreciation of the work done.
Impact Factor:
3.4 (2022);
5-Year Impact Factor:
3.5 (2022)
Latest Articles
Residual Cardiovascular Risk: Role of Remnants Cholesterol, Monocyte/HDL Ratio and Lipoprotein Ratios on Personalized Cardiovascular Prevention
J. Pers. Med. 2024, 14(5), 460; https://doi.org/10.3390/jpm14050460 - 26 Apr 2024
Abstract
Cardiovascular diseases represent the leading cause of death in the world and are subject to limitations in prevention strategies despite the use of very effective drugs. The concept of residual risk (RR) is intrinsically related to that of global risk of which it
[...] Read more.
Cardiovascular diseases represent the leading cause of death in the world and are subject to limitations in prevention strategies despite the use of very effective drugs. The concept of residual risk (RR) is intrinsically related to that of global risk of which it represents a very significant percentage. In the cardiovascular field, the term RR refers to the probability of incurring a major cardiovascular event, despite adequate control of the risk factors present in the individual patient. A significant portion of the RR in the cardiovascular field results from the underestimation of additional risk factors not subjected to adequate intervention such as, for example, triglyceride levels in patients treated for the presence of hypertension and/or hypercholesterolemia. The control of the RR therefore appears as an essential condition for the effective reduction of the global risk profile and is based on an integrated intervention that combines all the different prevention strategies derived from the available evidence and capable of interacting on the basis of a strengthening reciprocal between lifestyle and pharmacological and nutraceutical intervention methods.
Full article
(This article belongs to the Special Issue Advances in Diagnostics, Treatment and Management of Cardiovascular Diseases)
►
Show Figures
Open AccessArticle
Delayed Orbital Floor Reconstruction Using Mirroring Technique and Patient-Specific Implants: Proof of Concept
by
Diana D’Alpaos, Giovanni Badiali, Francesco Ceccariglia and Achille Tarsitano
J. Pers. Med. 2024, 14(5), 459; https://doi.org/10.3390/jpm14050459 - 26 Apr 2024
Abstract
Enophthalmos is a severe complication of primary reconstruction following orbital floor fractures, oncological resections, or maxillo-facial syndromes. The goal of secondary orbital reconstruction is to regain a symmetrical globe position to restore function and aesthetics. In this article, we present a method of
[...] Read more.
Enophthalmos is a severe complication of primary reconstruction following orbital floor fractures, oncological resections, or maxillo-facial syndromes. The goal of secondary orbital reconstruction is to regain a symmetrical globe position to restore function and aesthetics. In this article, we present a method of computer-assisted orbital floor reconstruction using a mirroring technique and a custom-made titanium or high-density polyethylene mesh printed using computer-aided manufacturing techniques. This reconstructive protocol involves four steps: mirroring of the healthy orbit computer tomography files at the contralateral affected site, virtual design of a customized implant, computer-assisted manufacturing (CAM) of the implant using Direct Metal Laser Sintering (DMLS) or Computer Numerical Control (CNC) methods, and surgical insertion of the device. Clinical outcomes were assessed using 3dMD photogrammetry and computed tomography measures in 13 treated patients and compared to a control group treated with stock implants. An improvement of 3.04 mm (range 0.3–6 mm) in globe protrusion was obtained for the patients treated with patient-specific implants (PSI), and no major complications have been registered. The technique described here appears to be a viable method for correcting complex orbital floor defects needing delayed reconstruction.
Full article
(This article belongs to the Section Methodology, Drug and Device Discovery)
►▼
Show Figures
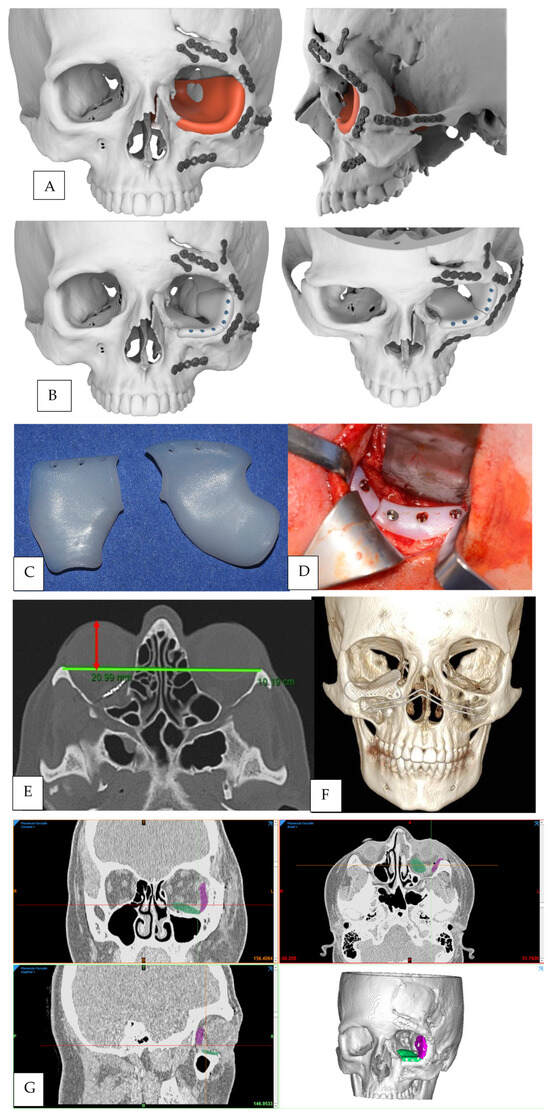
Figure 1
Open AccessArticle
Clinical Factors Affecting the Rate of Liver Regeneration in Living Donors after Right Hepatectomy
by
Minkyoung Kim, Suk-Won Suh, Eun Sun Lee, Sanggyun Suh, Seung Eun Lee and Yoo Shin Choi
J. Pers. Med. 2024, 14(5), 458; https://doi.org/10.3390/jpm14050458 - 26 Apr 2024
Abstract
Sufficient liver regeneration after a right hepatectomy is important in living donors for preventing postoperative hepatic insufficiency; however, it differs for each living donor so we investigated the clinical factors affecting the rate of liver regeneration after hepatic resection. This retrospective case–control study
[...] Read more.
Sufficient liver regeneration after a right hepatectomy is important in living donors for preventing postoperative hepatic insufficiency; however, it differs for each living donor so we investigated the clinical factors affecting the rate of liver regeneration after hepatic resection. This retrospective case–control study investigated fifty-four living donors who underwent a right hepatectomy from July 2015 to March 2023. Patients were classified into 2 groups by the remnant/total volume ratio (RTVR): Group A (RTVR < 30%, n = 9) and Group B (RTVR ≥ 30%, n = 45). The peak postoperative level of total bilirubin was more elevated in Group A than in Group B (3.0 ± 1.1 mg/dL vs. 2.3 ± 0.8 mg/dL, p = 0.046); however, no patients had hepatic insufficiency or major complications. The rates of residual liver volume (RLV) growth at Postoperative Week 1 (89.1 ± 26.2% vs. 53.5 ± 23.7%, p < 0.001) were significantly greater in Group A, and its significant predictors were RTVR (β = −0.478, p < 0.001, variance inflation factor (VIF) = 1.188) and intraoperative blood loss (β = 0.247, p = 0.038, VIF = 1.182). In conclusion, as the RLV decreases, compensatory liver regeneration after hepatic resection becomes more prominent, resulting in comparable operative outcomes. Further studies are required to investigate the relationship between hematopoiesis and the rate of liver regeneration.
Full article
(This article belongs to the Special Issue Personalized Medicine in Organ Transplantation 2nd Edition)
►▼
Show Figures
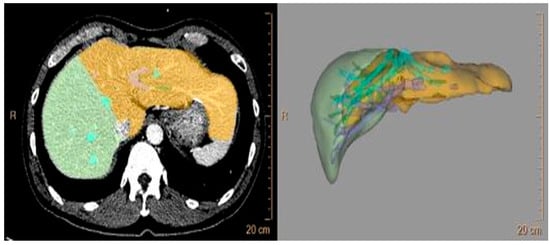
Figure 1
Open AccessArticle
Prognostic Value of KRAS Mutations in Relation to PDL1 Expression and Immunotherapy Treatment in Adenocarcinoma and Squamous Cell Carcinoma Patients: A Greek Cohort Study
by
Theodora Tsiouda, Kalliopi Domvri, Efimia Boutsikou, Vasileios Bikos, Krystallia Kyrka, Konstantina Papadaki, Persefoni Pezirkianidou, Konstantinos Porpodis and Angeliki Cheva
J. Pers. Med. 2024, 14(5), 457; https://doi.org/10.3390/jpm14050457 - 25 Apr 2024
Abstract
Background: Factors that could predict which patients will benefit from Immune Checkpoint Inhibitors (ICIs) are not fully understood. This study aimed to investigate the prognostic value of KRAS biomarker in patients with advanced non-small cell lung cancer (NSCLC) in relation to clinical characteristics,
[...] Read more.
Background: Factors that could predict which patients will benefit from Immune Checkpoint Inhibitors (ICIs) are not fully understood. This study aimed to investigate the prognostic value of KRAS biomarker in patients with advanced non-small cell lung cancer (NSCLC) in relation to clinical characteristics, treatment response and PDL1 expression. Patients and methods: The study included 100 patients with NSCLC who received immunotherapy with or without chemotherapy as 1st line treatment. In biopsy samples, the PDL1 biomarker expression rate and somatic mutations of KRAS gene were determined. Results: The mean age of the patients was 67 ± 8 years. Patients were all male and 66% were found with adenocarcinoma whereas 34% with squamous cell carcinoma. The KRAS G12C mutation was found with the highest percentage (73%). In the Kaplan-Meier survival analysis, patients with PDL1 > 49% in combination with a negative KRAS result had a median overall survival of 40 months compared to patients with a positive KRAS result (9 months, p < 0.05). In addition, patients diagnosed with adenocarcinoma, PDL1 < 49% and negative KRAS result had a median overall survival of 39 months compared to patients with a positive result (28 months, p < 0.05). Conclusions: Our study suggests that the presence of KRAS mutations in advanced NSCLC patients has a poor prognostic value, regardless of their PDL1 expression values, after receiving immunotherapy as first-line treatment.
Full article
(This article belongs to the Section Disease Biomarker)
Open AccessArticle
New Insight into Laryngo-Tracheal Surgery: High-Flow Oxygen Therapy to Prevent Early Complications after Surgery
by
Beatrice Trabalza Marinucci, Silvia Fiorelli, Alessandra Siciliani, Cecilia Menna, Matteo Tiracorrendo, Domenico Massullo, Federico Venuta, Erino Angelo Rendina, Anna Maria Ciccone, Antonio D’Andrilli, Mohsen Ibrahim and Giulio Maurizi
J. Pers. Med. 2024, 14(5), 456; https://doi.org/10.3390/jpm14050456 - 25 Apr 2024
Abstract
Background: Early post-operative airway management after laryngo-tracheal surgery is crucial. Acute respiratory failure due to glottis’ edema may occur, requiring reintubation. This can prolong ventilatory assistance, jeopardizing anastomosis. To date, only judicious steroid administration and fluid management are available to avoid more invasive
[...] Read more.
Background: Early post-operative airway management after laryngo-tracheal surgery is crucial. Acute respiratory failure due to glottis’ edema may occur, requiring reintubation. This can prolong ventilatory assistance, jeopardizing anastomosis. To date, only judicious steroid administration and fluid management are available to avoid more invasive procedures. High-flow oxygen therapy (HFOT) is a noninvasive O2 support method providing humidification, warmed air, and Positive End-Expiratory Pressure (AIRVO2). No data about HFOT use to prevent early complications after laryngo-tracheal surgery are reported in the literature. Methods: Between September 2020 and September 2022, 107 consecutive patients who underwent laryngo-tracheal surgery received HFOT (Group A). Data and long-term results were compared with those of 80 patients operated between September 2018 and August 2020 (Group B), when HFOT was not available. All patients were operated in a single center. No pre- or post-operative settings changed, except for HFOT introduction. We analyzed and compared the risk for “delayed” reintubation (unexpected reintubation within the first 24–48 h after extubating/laryngeal mask removal) in the two groups. Results: No patients reported HFOT-related adverse events. The control group (B) presented “delayed” reintubation in 37% (p = 0.027), intensive care unit admission in 67% (p = 0.005) and longer hospital stay (p = 0.001) compared to the HFOT group (A). The minor complications’ rate was 3% in both group and overall mortality was 0%. Re-stenosis was described in 4.6% of the HFOT group, without a statistically significant difference (p = 0.7006). Conclusions: Our study is the first to investigate HFOT use in patients undergoing laryngo-tracheal surgery, potentially representing a consistent innovation in the peri-operative management of these patients. With the limitation of a retrospective series, we would suggest HFOT use for preventing post-operative reintubation rate, possibly reducing ICU admissions and hospital stays.
Full article
(This article belongs to the Section Personalized Therapy and Drug Delivery)
Open AccessArticle
Assessing Maternal Satisfaction: Patient-Centered Care, Hospital Environment, and Information-Seeking in Chanika Hospital in Tanzania
by
Sarang Jang, Sangmi Lee and Aeree Sohn
J. Pers. Med. 2024, 14(5), 455; https://doi.org/10.3390/jpm14050455 - 25 Apr 2024
Abstract
This study examined the impact of patient-centered care, satisfaction with the hospital environment, and maternal information-seeking on maternal healthcare satisfaction in Tanzania. A total of 707 mothers who delivered at Chanika Hospital in Tanzania were surveyed using a structured questionnaire. Multiple regression analyses
[...] Read more.
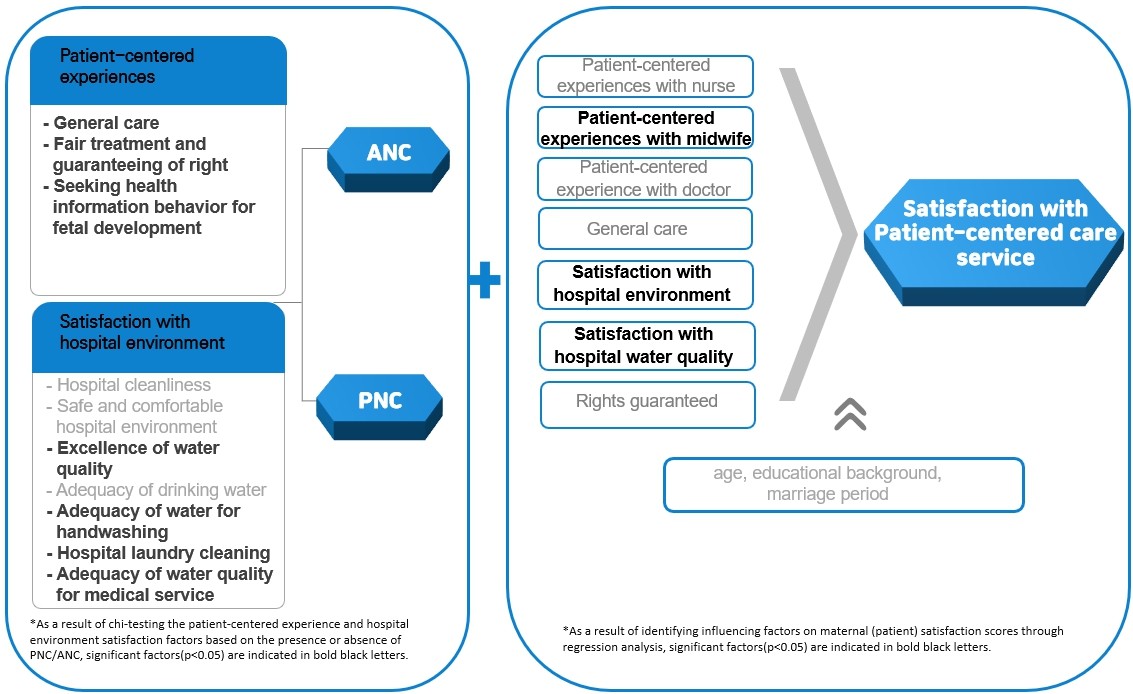
This study examined the impact of patient-centered care, satisfaction with the hospital environment, and maternal information-seeking on maternal healthcare satisfaction in Tanzania. A total of 707 mothers who delivered at Chanika Hospital in Tanzania were surveyed using a structured questionnaire. Multiple regression analyses were conducted to identify factors related to maternal satisfaction. Only 9.9% of the participants reported that they “usually” or “always” felt involved in treatment decisions. High levels of satisfaction were found for hospital cleanliness (93.6%) and safety (94.9%). However, there was a significant gap in satisfaction regarding the adequacy of water quality for medical services, with only 8.1% expressing satisfaction. Limited use of digital platforms was observed in terms of information-seeking behavior for fetal development, with only 19.5% of the participants using the internet and 14.3% using mobile apps. Patient-centered experiences with healthcare providers, especially midwives, had a significant positive impact on maternal satisfaction (β = 0.11, p = 0.021). Other significant variables were satisfaction with the hospital environment (β = 0.25, p < 0.001) and satisfaction with hospital water (β = 0.13, p < 0.001). It is recommended that healthcare improvements focus on patient-centered experiences and water quality for drinking and medical services to improve patient satisfaction.
Full article
(This article belongs to the Special Issue Patient-Centered Care for Chronic Diseases)
►▼
Show Figures
Graphical abstract
Open AccessArticle
The Role of Psychosomatic Traits in Tailored Workup for Anterior Cervical Discectomy and Fusion—A Case Series
by
Marco Battistelli, Edoardo Mazzucchi, Mario Muselli, Filippo Maria Polli, Gianluca Galieri, Paola Bazzu, Fabrizio Pignotti, Alessandro Olivi, Giovanni Sabatino and Giuseppe La Rocca
J. Pers. Med. 2024, 14(5), 454; https://doi.org/10.3390/jpm14050454 - 25 Apr 2024
Abstract
Study design: Prospective study. Objective: To evaluate the influence of preoperatively assessed psychosomatic traits on postoperative pain, disability, and quality of life outcomes. Summary of background data: Anterior cervical discectomy and fusion (ACDF) is a widely employed surgical procedure for treating cervical spondylosis.
[...] Read more.
Study design: Prospective study. Objective: To evaluate the influence of preoperatively assessed psychosomatic traits on postoperative pain, disability, and quality of life outcomes. Summary of background data: Anterior cervical discectomy and fusion (ACDF) is a widely employed surgical procedure for treating cervical spondylosis. Despite its effectiveness, various studies have reported non-success rates in terms of alleviating disability and pain. Psychological factors have become increasingly recognized as critical determinants of surgical outcomes in various medical disciplines. The full extent of their impact within the context of ACDF remains insufficiently explored. This case series aims to assess the influence of preoperative psychological profiling on long-term pain, disability and quality of life outcomes. Methods: We conducted a prospective cohort study of prospectively collected data from 76 consecutive patients who underwent ACDF with PEEK inter-fixed cages from July 2019 to November 2021. The preoperative psychological traits were assessed using the Symptom Checklist 90 (SCL-90) questionnaire. The Oswestry Disability Index (ODI), Visual Analogue Scale (VAS), Neck Disability index (NDI), EuroQol-5D (EQ-5D), and Short Form-36 (SF-36) were collected preoperatively, one month postoperatively, and at least one year after the surgical procedure. Results: The correlation analyses revealed associations between psychosomatic traits and multiple preoperative and postoperative outcome measures. The univariate analyses and linear regression analyses demonstrated the influence of the Global Severity Index (GSI) over the final follow-up scores for the ODI, VAS, NDI, EQ-5D, and SF-36. The GSI consistently exhibited a stronger correlation with the final follow-up pain, disability, and quality of life outcomes with respect to the correspondent preoperative values. Conclusion: This study highlights the importance of psychosomatic traits as predictive factors for ACDF outcomes and emphasizes their relevance in preoperative assessment for informing patients about realistic expectations. The findings underscore the need to consider psychological profiles in the preoperative workup, opening avenues for research into medications and psychological therapies. Recognizing the influence of psychosocial elements informs treatment strategies, fostering tailored surgical approaches and patient care.
Full article
(This article belongs to the Special Issue Precision Medicine in Neurosurgery)
Open AccessArticle
The Causal Effect of Gut Microbiota and Plasma Metabolome on Lung Cancer and the Heterogeneity across Subtypes: A Mendelian Randomization Study
by
Jun Zeng, Bin Yi, Ruimin Chang, Jiashuo Li, Jiebo Zhu, Zhongjie Yu, Xi Li and Yang Gao
J. Pers. Med. 2024, 14(5), 453; https://doi.org/10.3390/jpm14050453 - 25 Apr 2024
Abstract
The causal effect and pathways of gut microbiota and plasma metabolome on lung cancer have been important topics for personalized medicine; however, the heterogeneity of lung cancer subtypes has not gained enough attention in previous studies. This study sought to employ a Mendelian
[...] Read more.
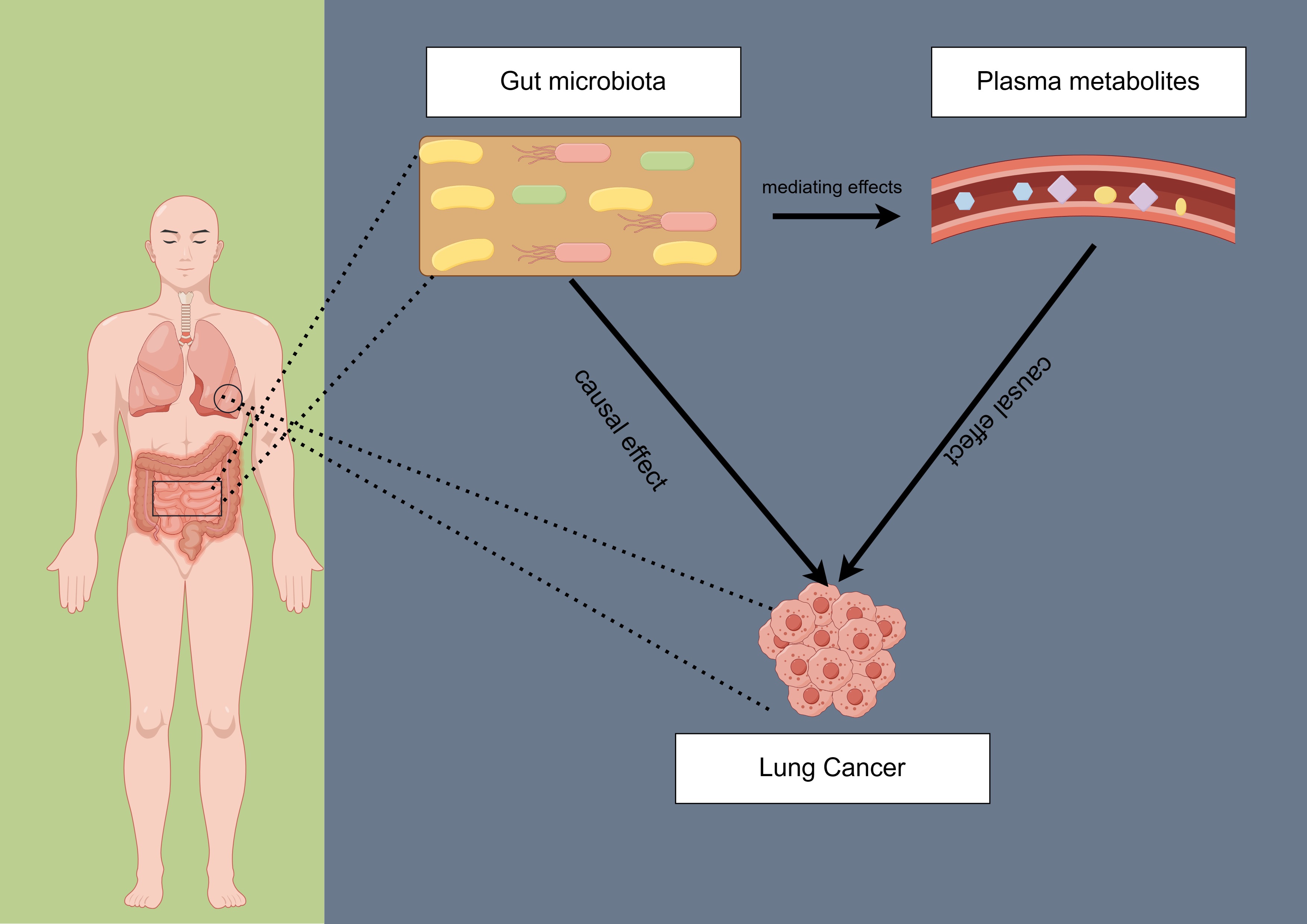
The causal effect and pathways of gut microbiota and plasma metabolome on lung cancer have been important topics for personalized medicine; however, the heterogeneity of lung cancer subtypes has not gained enough attention in previous studies. This study sought to employ a Mendelian randomization analysis to screen the specific gut microbiota and plasma metabolome, which may have a causal effect on lung cancer. We further extended our analysis to estimate the effects of these exposures on various pathological subtypes of lung cancer. Furthermore, a mediation analysis was performed to identify the potential pathway underlying the influence of microbiota and metabolites. Our study identified 13 taxa and 15 metabolites with a causal association with the overall risk of lung cancer. Furthermore, we found 8 taxa and 14 plasma metabolites with a causal effect on lung adenocarcinoma, 4 taxa and 10 metabolites with a causal effect on squamous cell lung carcinoma, and 7 taxa and 16 metabolites with a causal effect on SCLC. We also identified seven mediation pathways that could potentially elucidate the influence of these microbiota and metabolites on overall lung cancer or special subtypes. Our study highlighted the heterogeneity of the gut microbiome and plasma metabolome in a lung cancer subtype and elucidated the potential underlying mechanisms. This could pave the way for more personalized lung cancer prevention and treatment.
Full article
(This article belongs to the Special Issue The Correlation between Gut Microbiota and Cancers)
►▼
Show Figures
Graphical abstract
Open AccessReview
Preoperative Ultrasound for the Prediction of Postinduction Hypotension: A Systematic Review and Meta-Analysis
by
Chunyu Liu, Ran An and Hongliang Liu
J. Pers. Med. 2024, 14(5), 452; https://doi.org/10.3390/jpm14050452 - 25 Apr 2024
Abstract
Postinduction hypotension (PIH) is closely associated with postoperative adverse outcomes. Preoperative hypovolemia is a key risk factor, and many parameters are available from ultrasound to detect hypovolemia, but the accuracy of PIH from ultrasound remains unclear. This systematic review and meta-analysis aimed to
[...] Read more.
Postinduction hypotension (PIH) is closely associated with postoperative adverse outcomes. Preoperative hypovolemia is a key risk factor, and many parameters are available from ultrasound to detect hypovolemia, but the accuracy of PIH from ultrasound remains unclear. This systematic review and meta-analysis aimed to evaluate the commonly used measurements from ultrasound to predict PIH. We searched the PubMed, Cochrane Library, Embase, CNKI, and Web of Science databases from their inception to December 2023. Thirty-six studies were included for quantitative analysis. The pooled sensitivities for the inferior vena cava collapsibility index (IVC-CI), maximum inferior vena cava diameter (DIVCmax), minimum inferior vena cava diameter (DIVCmin), and carotid artery corrected flow time (FTc) were 0.73 (95% CI = 0.65, 0.79), 0.66 (95% CI = 0.54, 0.77), 0.74 (95% CI = 0.60, 0.85), and 0.81 (95% CI = 0.72, 0.88). The pooled specificities for the IVC-CI, DIVCmax, DIVCmin, and carotid artery FTc were 0.82 (95% CI = 0.75, 0.87), 0.75 (95% CI = 0.66, 0.82), 0.76 (95% CI = 0.65, 0.84), and 0.87 (95% CI = 0.77, 0.93). The AUC for the IVC-CI, DIVCmax, DIVCmin, and carotid artery FTc were 0.84 (95% CI = 0.81, 0.87), 0.77 (95% CI = 0.73, 0.81), 0.82 (95% CI = 0.78, 0.85), and 0.91 (95% CI = 0.88, 0.93). Our study demonstrated that ultrasound indices are reliable predictors for PIH. The carotid artery FTc is probably the optimal ultrasound measurement for identifying patients who will develop PIH in our study.
Full article
(This article belongs to the Special Issue Precision Emergency Medicine)
►▼
Show Figures
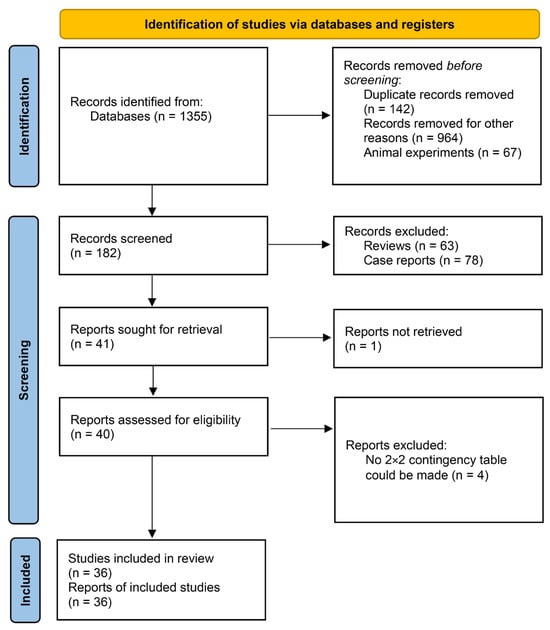
Figure 1
Open AccessArticle
Restoration of Pulmonary Compliance after Laparoscopic Gynecologic Surgery Using a Recruitment Maneuver
by
Panagiota Griva, Christina Talliou, Loizos Rougeris, Dimitra Samara, Konstantina Panagouli, Giolanda Varvarousi, Maria Papa, Nikolaos Kathopoulis, Vasiliki Chantziara and Nikoletta Rovina
J. Pers. Med. 2024, 14(5), 451; https://doi.org/10.3390/jpm14050451 - 25 Apr 2024
Abstract
Background/Objectives: This study aimed to investigate the hypothesis that an alveolar recruitment maneuver can restore lung compliance to initial values after laparoscopic gynecological surgery. Methods: A total of 31 patients who underwent laparoscopic gynecological surgery were enrolled. Protective mechanical ventilation was applied, and
[...] Read more.
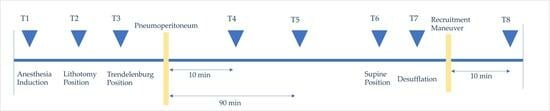
Background/Objectives: This study aimed to investigate the hypothesis that an alveolar recruitment maneuver can restore lung compliance to initial values after laparoscopic gynecological surgery. Methods: A total of 31 patients who underwent laparoscopic gynecological surgery were enrolled. Protective mechanical ventilation was applied, and the radial artery was catheterized in all patients. An alveolar recruitment maneuver (incremental and decremental positive end-expiratory pressure) was applied ten minutes after the release of pneumoperitoneum. The respiratory mechanics and blood gas results were recorded at eight different time points: after induction of anesthesia (T1), in the lithotomy position (T2), in the Trendelenburg position (T3), 10 and 90 min after insufflation of carbon dioxide (T4 and T5), in the supine position (T6), after desufflation (T7), and 10 min after an alveolar recruitment maneuver at the end of surgery (T8). Results: Pneumoperitoneum and the Trendelenburg position caused a decline of 15 units in compliance (T7 vs. T1; p < 0.05) compared to baseline. After the alveolar recruitment maneuver, compliance increased by 17.5% compared with the mean value of compliance at time T1 (T8 vs. T1; p < 0.05). The recruitment maneuver had favorable results in patients with low initial compliance (41.5 mL/cmH2O, IQR: 9.75 mL/cmH2O), high Body Mass Index 30.32 kg/m2 (IQR: 1.05 kg/m2), and high initial plateau airway pressure (16.5 cmH2O, IQR: 0.75 cmH2O). Conclusions: Lung compliance does not return to initial values after performing laparoscopic gynecological procedures. However, after the release of pneumoperitoneum, an alveolar recruitment maneuver is beneficial as it improves compliance and gas exchange.
Full article
(This article belongs to the Special Issue Obstetrics and Gynecology and Women's Health)
►▼
Show Figures
Graphical abstract
Open AccessArticle
Evaluation of a 3D Printed Silicone Oral Cavity Cancer Model for Surgical Simulations
by
Donovan Eu, Michael J. Daly, Stefano Taboni, Axel Sahovaler, Ashley N. Gilbank and Jonathan C. Irish
J. Pers. Med. 2024, 14(5), 450; https://doi.org/10.3390/jpm14050450 - 25 Apr 2024
Abstract
Adequate surgical margins are essential in oral cancer treatment, this is, however, difficult to appreciate during training. With advances in training aids, we propose a silicone-based surgical simulator to improve training proficiency for the ablation of oral cavity cancers. A silicone-based tongue cancer
[...] Read more.
Adequate surgical margins are essential in oral cancer treatment, this is, however, difficult to appreciate during training. With advances in training aids, we propose a silicone-based surgical simulator to improve training proficiency for the ablation of oral cavity cancers. A silicone-based tongue cancer model constructed via a 3D mold was compared to a porcine tongue model used as a training model. Participants of varying surgical experience were then asked to resect the tumors with clear margins, and thereafter asked to fill out a questionnaire to evaluate the face and content validity of the models as a training tool. Eleven participants from the Otolaryngology-Head and Neck Surgery unit were included in this pilot study. In comparison to the porcine model, the silicone model attained a higher face (4 vs. 3.6) and content validity (4.4 vs. 4.1). Tumor consistency was far superior in the silicone model compared to the porcine model (4.1 vs. 2.8, p = 0.0042). Fellows and staff demonstrated a better margin clearance compared to residents (median 3.5 mm vs. 1.0 mm), and unlike the resident group, there was no incidence of positive margins. The surgical simulation was overall useful for trainees to appreciate the nature of margin clearance in oral cavity cancer ablation.
Full article
(This article belongs to the Special Issue Precision Medicine for Head and Neck Surgery)
►▼
Show Figures
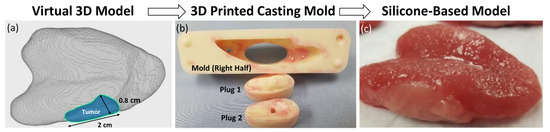
Figure 1
Open AccessArticle
Naïve Inflammatory Proteome Profiles of Glucocorticoid Responsive Polymyalgia Rheumatica and Rheumatic Arthritis Patients—Links to Triggers and Proteomic Manifestations
by
Allan Stensballe, Jacob Skallerup Andersen, Christopher Aboo, Anders Borg Andersen, Jie Ren, Michael Kruse Meyer, Kate Lykke Lambertsen and Peter Derek Christian Leutscher
J. Pers. Med. 2024, 14(5), 449; https://doi.org/10.3390/jpm14050449 - 25 Apr 2024
Abstract
Polymyalgia rheumatica (PMR) is an inflammatory disorder of unknown etiology, sharing symptoms with giant cell arthritis (GCA) and rheumatoid arthritis (RA). The pathogenic inflammatory roots are still not well understood, and there is a lack of extensive biomarker studies to explain the disease
[...] Read more.
Polymyalgia rheumatica (PMR) is an inflammatory disorder of unknown etiology, sharing symptoms with giant cell arthritis (GCA) and rheumatoid arthritis (RA). The pathogenic inflammatory roots are still not well understood, and there is a lack of extensive biomarker studies to explain the disease debut and post-acute phase. This study aimed to deeply analyze the serum proteome and inflammatory response of PMR patients before and after glucocorticoid treatment. We included treatment-naïve PMR patients, collecting samples before and after 3 months of treatment. For comparison, disease-modifying antirheumatic drug (DMARD)-naïve RA patients were included and matched to healthy controls (CTL). The serum proteome was examined using label-free quantitative mass spectrometry, while inflammation levels were assessed using multiplex inflammatory cytokine and cell-free DNA assays. The serum proteomes of the four groups comprised acute phase reactants, coagulation factors, complement proteins, immunoglobulins, and apolipoproteins. Serum amyloid A (SAA1) was significantly reduced by active PMR treatment. Cell-free DNA levels in PMR and RA groups were significantly higher than in healthy controls due to acute inflammation. Complement factors had minimal changes post-treatment. The individual serum proteome in PMR patients showed over 100 abundantly variable proteins, emphasizing the systemic impact of PMR disease debut and the effect of treatment. Interleukin (IL)-6 and interferon-gamma (IFN-γ) were significantly impacted by glucocorticoid treatment. Our study defines the PMR serum proteome during glucocorticoid treatment and highlights the role of SAA1, IL-6, and IFN-γ in treatment responses. An involvement of PGLYRP2 in acute PMR could indicate a response to bacterial infection, highlighting its role in the acute phase of the immune response. The results suggest that PMR may be an aberrant response to a bacterial infection with an exacerbated IL-6 and acute phase inflammatory response and molecular attempts to limit the inflammation.
Full article
(This article belongs to the Special Issue Personalized Medicine in Rheumatology—towards Adapting Our Care to Manifold Patient Phenotypes)
►▼
Show Figures
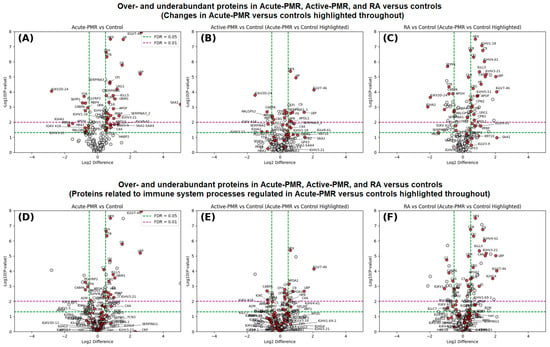
Figure 1
Open AccessArticle
Automated Evaluation of Ellipsoid Zone At-Risk Burden for Detection of Hydroxychloroquine Retinopathy
by
Katherine E. Talcott, Gagan Kalra, Hasan Cetin, Yavuz Cakir, Jon Whitney, Jordan Budrevich, Jamie L. Reese, Sunil K. Srivastava and Justis P. Ehlers
J. Pers. Med. 2024, 14(5), 448; https://doi.org/10.3390/jpm14050448 - 25 Apr 2024
Abstract
Background: Screening for hydroxychloroquine (HCQ) retinopathy is crucial to detecting early disease. A novel machine-learning-based optical coherence tomography (OCT) biomarker, Ellipsoid Zone (EZ) At-Risk, can quantitatively measure EZ alterations and at-risk areas for progressive EZ loss in a fully automated fashion. The purpose
[...] Read more.
Background: Screening for hydroxychloroquine (HCQ) retinopathy is crucial to detecting early disease. A novel machine-learning-based optical coherence tomography (OCT) biomarker, Ellipsoid Zone (EZ) At-Risk, can quantitatively measure EZ alterations and at-risk areas for progressive EZ loss in a fully automated fashion. The purpose of this analysis was to compare the EZ At-Risk burden in eyes with HCQ toxicity to eyes without toxicity. Methods: IRB-approved image analysis study of 83 subjects on HCQ and 44 age-matched normal subjects. SD-OCT images were reviewed for evidence of HCQ retinopathy. A ML-based, fully automatic measurement of the percentage of the macular area with EZ At-Risk was performed. Results: The mean age for HCQ subjects was 67.1 ± 13.2 years and 64.2 ± 14.3 years for normal subjects. The mean EZ At-Risk macular burden in the “toxic” group (n = 38) was significantly higher (10.7%) compared to the “non-toxic” group (n = 45; 2.2%; p = 0.023) and the “normal” group (1.4%; p = 0.012). Additionally, the amount of EZ At-Risk burden was significantly correlated with the HCQ dose based on the actual (p = 0.016) and ideal body weight (p = 0.033). Conclusions: The novel biomarker EZ-At Risk was significantly higher in subjects with evidence of HCQ retinopathy as well as significantly associated with HCQ dose. This novel biomarker should be further evaluated as a potential screening tool for subjects on HCQ.
Full article
(This article belongs to the Special Issue Imaging Biomarkers for Retinal Diseases: Prognostic Tools and Novel Clinical Trial Endpoints for Precision Medicine)
►▼
Show Figures
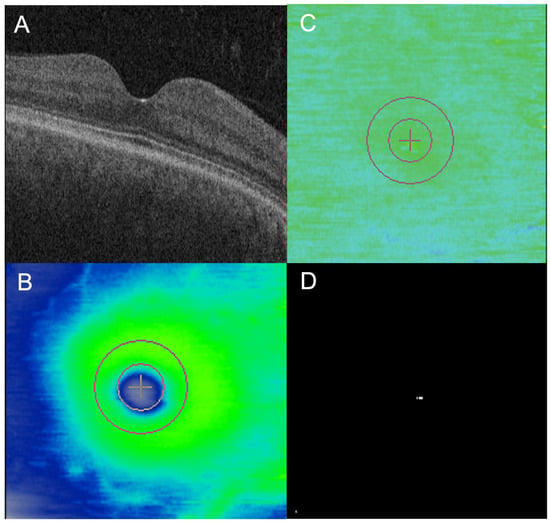
Figure 1
Open AccessArticle
Attitudes of Jordanian Anesthesiologists and Anesthesia Residents towards Artificial Intelligence: A Cross-Sectional Study
by
Isam Bsisu, Rami Alqassieh, Abdelkarim Aloweidi, Abdulrahman Abu-Humdan, Aseel Subuh and Deema Masarweh
J. Pers. Med. 2024, 14(5), 447; https://doi.org/10.3390/jpm14050447 - 25 Apr 2024
Abstract
Success in integrating artificial intelligence (AI) in anesthesia depends on collaboration with anesthesiologists, respecting their expertise, and understanding their opinions. The aim of this study was to illustrate the confidence in AI integration in perioperative anesthetic care among Jordanian anesthesiologists and anesthesia residents
[...] Read more.
Success in integrating artificial intelligence (AI) in anesthesia depends on collaboration with anesthesiologists, respecting their expertise, and understanding their opinions. The aim of this study was to illustrate the confidence in AI integration in perioperative anesthetic care among Jordanian anesthesiologists and anesthesia residents working at tertiary teaching hospitals. This cross-sectional study was conducted via self-administered online questionnaire and includes 118 responses from 44 anesthesiologists and 74 anesthesia residents. We used a five-point Likert scale to investigate the confidence in AI’s role in different aspects of the perioperative period. A significant difference was found between anesthesiologists and anesthesia residents in confidence in the role of AI in operating room logistics and management, with an average score of 3.6 ± 1.3 among residents compared to 2.9 ± 1.4 among specialists (p = 0.012). The role of AI in event prediction under anesthesia scored 3.5 ± 1.4 among residents compared to 2.9 ± 1.4 among specialists (p = 0.032) and the role of AI in decision-making in anesthetic complications 3.3 ± 1.4 among residents and 2.8 ± 1.4 among specialists (p = 0.034). Also, 65 (55.1%) were concerned that the integration of AI will lead to less human–human interaction, while 81 (68.6%) believed that AI-based technology will lead to more adherence to guidelines. In conclusion, AI has the potential to be a revolutionary tool in anesthesia, and hesitancy towards increased dependency on this technology is decreasing with newer generations of practitioners.
Full article
(This article belongs to the Section Personalized Critical Care)
Open AccessReview
Enhancing Lung Cancer Care in Portugal: Bridging Gaps for Improved Patient Outcomes
by
Raquel Ramos, Conceição Souto Moura, Mariana Costa, Nuno Jorge Lamas, Renato Correia, Diogo Garcez, José Miguel Pereira, Carlos Sousa and Nuno Vale
J. Pers. Med. 2024, 14(5), 446; https://doi.org/10.3390/jpm14050446 - 24 Apr 2024
Abstract
Lung cancer has the highest incidence and cancer-related mortality worldwide. In Portugal, it ranks as the fourth most common cancer, with nearly 6000 new cases being diagnosed every year. Lung cancer is the main cause of cancer-related death among males and the third
[...] Read more.
Lung cancer has the highest incidence and cancer-related mortality worldwide. In Portugal, it ranks as the fourth most common cancer, with nearly 6000 new cases being diagnosed every year. Lung cancer is the main cause of cancer-related death among males and the third cause of cancer-related death in females. Despite the globally accepted guidelines and recommendations for what would be the ideal path for a lung cancer patient, several challenges occur in real clinical management across the world. The recommendations emphasize the importance of adequate screening of high-risk individuals, a precise tumour biopsy, and an accurate final diagnosis to confirm the neoplastic nature of the nodule. A detailed histological classification of the lung tumour type and a comprehensive molecular characterization are of utmost importance for the selection of an efficacious and patient-directed therapeutic approach. However, in the context of the Portuguese clinical organization and the national healthcare system, there are still several gaps in the ideal pathway for a lung cancer patient, involving aspects ranging from the absence of a national lung cancer screening programme through difficulties in histological diagnosis and molecular characterization to challenges in therapeutic approaches. In this manuscript, we address the most relevant weaknesses, presenting several proposals for potential solutions to improve the management of lung cancer patients, helping to decisively improve their overall survival and quality of life.
Full article
(This article belongs to the Section Personalized Critical Care)
Open AccessArticle
Nerve Regeneration after a Nerve Graft in a Rat Model: The Effectiveness of Fibrin Glue
by
Giovanni Zabbia, Francesca Toia, Federico Coppola, Giovanni Cassata, Luca Cicero, Giuseppe Giglia, Roberto Puleio and Adriana Cordova
J. Pers. Med. 2024, 14(5), 445; https://doi.org/10.3390/jpm14050445 - 24 Apr 2024
Abstract
Background: Simulating the post-traumatic continuity defect of small human peripheral nerves, we compared the effectiveness of fibrin glue with neurorrhaphy for nerve gap restoration. Methods: In twenty-four male Wistar rats, a fifteen mm defect in one sciatic nerve only was made and immediately
[...] Read more.
Background: Simulating the post-traumatic continuity defect of small human peripheral nerves, we compared the effectiveness of fibrin glue with neurorrhaphy for nerve gap restoration. Methods: In twenty-four male Wistar rats, a fifteen mm defect in one sciatic nerve only was made and immediately repaired with an inverted polarity autograft. According to the used technique, rats were divided into Group A (Control), using traditional neurorrhaphy, and Group B (Study), using fibrine glue sealing; in total, 50% of rats were sacrificed at 16 weeks and 50% at 21 weeks. Before sacrifice, an assessment of motor function was done through Walking Track Analysis and an electroneurophysiological evaluation. After sacrifice, selected muscle mass indexes and the histology of the regenerated nerves were assessed. All data were evaluated by Student’s t test for unpaired data. Results: No significant differences were found between the two groups, with only the exception of a relative improvement in the tibialis anterior muscle’s number of motor units in the study group. Conclusion: Despite the fact that the use of fibrin glue as a nerve sealant is not superior in terms of functional recovery, its effectiveness is comparable to that of microsurgical repair. Hence, the faster and technically easier glueing technique could deserve broader clinical application.
Full article
(This article belongs to the Section Regenerative Medicine and Therapeutics)
Open AccessArticle
Real-Life Prognosis of Sinonasal Tumors
by
Giancarlo Pecorari, Gian Marco Motatto, Federica Piazza, Alessandro Garzaro and Giuseppe Riva
J. Pers. Med. 2024, 14(5), 444; https://doi.org/10.3390/jpm14050444 - 24 Apr 2024
Abstract
Background: Sinonasal cancer represents a challenging disease because of its difficult diagnosis and different histology. Despite a multidisciplinary evaluation and treatments, a poor prognosis is still present. We retrospectively analyzed patients with sinonasal cancer treated in our institution, paying attention to histology and
[...] Read more.
Background: Sinonasal cancer represents a challenging disease because of its difficult diagnosis and different histology. Despite a multidisciplinary evaluation and treatments, a poor prognosis is still present. We retrospectively analyzed patients with sinonasal cancer treated in our institution, paying attention to histology and real-life prognosis. Methods: A total of 51 consecutive patients were included in the study. Clinical features were described. Overall, disease-free, and disease-specific survival (OS, DFS, DSS) according to histology were calculated. Kaplan–Meyer estimator curves were reported. Results: The most prevalent primary tumor was squamous cell carcinoma, followed by adenocarcinoma. Global 2- and 5-year OS was 68.80% and 54.58%, respectively. Global 2- and 5-year DFS was 48.53% and 29.56%, while global 2- and 5-year DSS was 82.86% and 74.57%, respectively. The median OS was 74 and 43 months for early- and late-stage cancer, respectively. The Cox multivariate regression analysis did not reveal any statistically significant effects of age, stage, or histology on survival outcomes. Conclusions: The diagnosis is often late and the prognosis poor. An appropriate treatment, which is always quite multimodal, allows us to achieve a global 5-year OS slightly higher than 50%. An adequate diagnosis to increase the percentage of early-stage tumors is mandatory to improve prognosis.
Full article
(This article belongs to the Special Issue Current Status and Future Research in Otorhinolaryngology)
►▼
Show Figures

Figure 1
Open AccessReview
Clearing the Fog: A Scoping Literature Review on the Ethical Issues Surrounding Artificial Intelligence-Based Medical Devices
by
Alessia Maccaro, Katy Stokes, Laura Statham, Lucas He, Arthur Williams, Leandro Pecchia and Davide Piaggio
J. Pers. Med. 2024, 14(5), 443; https://doi.org/10.3390/jpm14050443 - 23 Apr 2024
Abstract
The use of AI in healthcare has sparked much debate among philosophers, ethicists, regulators and policymakers who raised concerns about the implications of such technologies. The presented scoping review captures the progression of the ethical and legal debate and the proposed ethical frameworks
[...] Read more.
The use of AI in healthcare has sparked much debate among philosophers, ethicists, regulators and policymakers who raised concerns about the implications of such technologies. The presented scoping review captures the progression of the ethical and legal debate and the proposed ethical frameworks available concerning the use of AI-based medical technologies, capturing key themes across a wide range of medical contexts. The ethical dimensions are synthesised in order to produce a coherent ethical framework for AI-based medical technologies, highlighting how transparency, accountability, confidentiality, autonomy, trust and fairness are the top six recurrent ethical issues. The literature also highlighted how it is essential to increase ethical awareness through interdisciplinary research, such that researchers, AI developers and regulators have the necessary education/competence or networks and tools to ensure proper consideration of ethical matters in the conception and design of new AI technologies and their norms. Interdisciplinarity throughout research, regulation and implementation will help ensure AI-based medical devices are ethical, clinically effective and safe. Achieving these goals will facilitate successful translation of AI into healthcare systems, which currently is lagging behind other sectors, to ensure timely achievement of health benefits to patients and the public.
Full article
(This article belongs to the Special Issue Artificial Intelligence Applied to Clinical Practice)
►▼
Show Figures
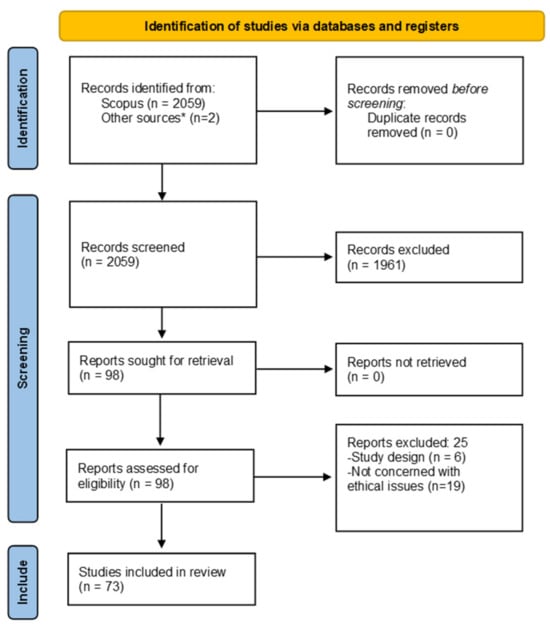
Figure 1
Open AccessArticle
Isolated Limb Perfusion and Immunotherapy in the Treatment of In-Transit Melanoma Metastases: Is It a Real Synergy?
by
Marco Rastrelli, Francesco Russano, Francesco Cavallin, Paolo Del Fiore, Claudia Pacilli, Claudia Di Prata, Carlo Riccardo Rossi, Antonella Vecchiato, Luigi Dall’Olmo and Simone Mocellin
J. Pers. Med. 2024, 14(5), 442; https://doi.org/10.3390/jpm14050442 - 23 Apr 2024
Abstract
Background: Isolated limb hyperthermic-antiblastic perfusion (ILP) was the most effective local treatment for advanced in-transit melanoma, but the advent of modern effective immunotherapy (IT), such as immune checkpoint inhibitors, has changed the treatment landscape. Methods: This study evaluated the role of the association
[...] Read more.
Background: Isolated limb hyperthermic-antiblastic perfusion (ILP) was the most effective local treatment for advanced in-transit melanoma, but the advent of modern effective immunotherapy (IT), such as immune checkpoint inhibitors, has changed the treatment landscape. Methods: This study evaluated the role of the association between ILP and IT in the treatment of locally advanced unresectable melanoma, particularly in relation to modern systemic therapies. We analyzed 187 consecutive patients who were treated with ILP (melphalan or melphalan associated with TNF-alpha) for advanced melanoma at the Veneto Institute of Oncology of Padua (Italy) and the Padua University Hospital (Italy) between June 1989 and September 2021. Overall survival (OS), disease-specific survival (DSS), local disease-free survival (local DFS) and distant disease-free survival (distant DFS) were evaluated. Local toxicity was classified according to the Wieberdink scale and surgical complications according to the Clavien–Dindo classification. Response to locoregional therapy was evaluated during follow-up according to the RECIST 1.1 criteria (Response Evaluation Criteria in Solid Tumor). Results: A total of 99 patients were treated with ILP and 88 with IT + ILP. The overall response rate was 67% in both groups. At 36 months, OS was 43% in the ILP group and 61% in the ILP + IT group (p = 0.02); DSS was 43% in the ILP group and 64% in the ILP + IT group (p = 0.02); local DFS was the 37% in ILP group and 53% in the ILP + IT group (p = 0.04); and distant DFS was 33% in the ILP group and 35% in the ILP + IT group (p = 0.40). Adjusting for age and lymph node involvement, receiving ILP + IT was associated with improved OS (p = 0.01) and DSS (p = 0.007) but not local DFS (p = 0.13) and distant DFS (p = 0.21). Conclusions: Our findings confirm the synergy between ILP and IT. ILP remains a valuable loco-regional treatment option in the era of effective systemic treatments. Further studies are needed to establish the optimal combination of loco-regional and systemic treatments and address the best timing of this combination to obtain the highest local response rate.
Full article
(This article belongs to the Special Issue New Insights into Personalized Surgical Oncology)
►▼
Show Figures
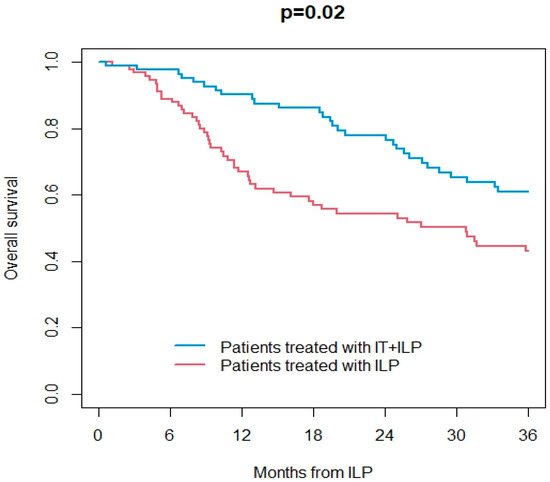
Figure 1
Open AccessArticle
Efficacy of Single- and Dual-Docking Robotic Surgery of Paraaortic and Pelvic Lymphadenectomy in High-Risk Endometrial Cancer
by
Magdalena Bizoń, Maciej Olszewski, Agnieszka Grabowska, Joanna Siudek, Krzysztof Mawlichanów and Radovan Pilka
J. Pers. Med. 2024, 14(5), 441; https://doi.org/10.3390/jpm14050441 - 23 Apr 2024
Abstract
(1) The surgical method of choice for the treatment of endometrial cancer is minimally invasive surgery. In cases of high-risk endometrial cancer, completed paraaortic and pelvic lymphadenectomy are indicated. The aim of this study was to analyze the types of docking during robotic
[...] Read more.
(1) The surgical method of choice for the treatment of endometrial cancer is minimally invasive surgery. In cases of high-risk endometrial cancer, completed paraaortic and pelvic lymphadenectomy are indicated. The aim of this study was to analyze the types of docking during robotic surgery assisted with the da Vinci X system while performing paraaortic and pelvic lymphadenectomy. (2) Methods: A total of 25 patients with high-risk endometrial cancer, with a mean age of 60.07 ± 10.67 (range 34.69–83.23) years, and with a mean body mass index (BMI) of 28.4 ± 5.62 (range 18–41.5) kg/m2, were included in this study. The analyzed population was divided into groups that underwent single or dual docking during surgery. (3) Results: No statistical significance was observed between single and dual docking during paraaortic and pelvic lymphadenectomy and between the type of docking and the duration of the operation. However, there was a statistically significant correlation between the duration of the operation and previous surgery (p < 0.005). The number of removed lymph nodes was statistically associated with BMI (p < 0.005): 15.87 ± 6.83 and 24.5 ± 8.7 for paraaortic and pelvic lymph nodes, respectively, in cases of single docking, and 18.05 ± 7.92 and 24.88 ± 11.75 for paraaortic and pelvic lymph nodes, respectively, in cases of dual docking. (4) Conclusions: The robot-assisted approach is a good surgical method for lymphadenectomy for obese patients, and, despite the type of docking, there are no differences in the quality of surgery.
Full article
(This article belongs to the Special Issue Advanced Minimally Invasive Surgery in Gynecology: Second Edition)
►▼
Show Figures
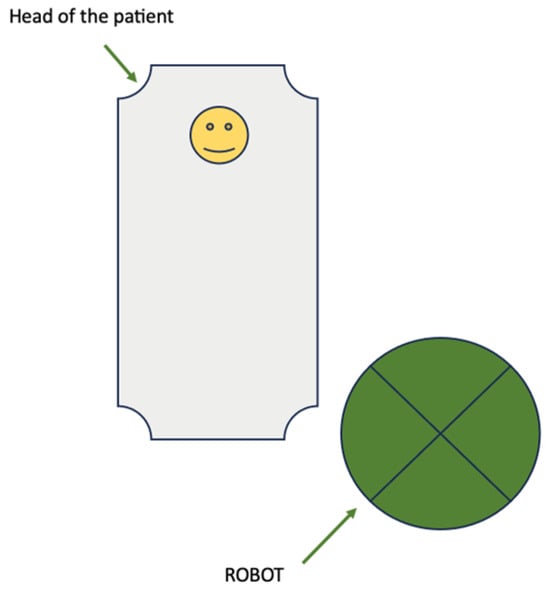
Figure 1

Journal Menu
► ▼ Journal Menu-
- JPM Home
- Aims & Scope
- Editorial Board
- Reviewer Board
- Topical Advisory Panel
- Instructions for Authors
- Special Issues
- Topics
- Sections & Collections
- Article Processing Charge
- Indexing & Archiving
- Editor’s Choice Articles
- Most Cited & Viewed
- Journal Statistics
- Journal History
- Journal Awards
- Conferences
- Editorial Office
Journal Browser
► ▼ Journal BrowserHighly Accessed Articles
Latest Books
E-Mail Alert
News
Topics
Topic in
Biomolecules, Diagnostics, JCM, Metabolites, JPM, Nutrients
Metabolic Syndrome, Biomarkers and Lifestyles
Topic Editors: Sang Yeoup Lee, Young Hye ChoDeadline: 30 June 2024
Topic in
Biomedicines, JCM, JPM
Current Challenges and Advances in Skin Repair and Regeneration
Topic Editors: Giovanni Salzano, Chiara CopelliDeadline: 20 July 2024
Topic in
Clinics and Practice, JCM, JPM, Healthcare, Diagnostics
Pathology and Current State of Treatment of Chronic Pain
Topic Editors: Tatsunori Ikemoto, Young-Chang AraiDeadline: 31 July 2024
Topic in
Antibiotics, JPM, Pharmaceuticals, Pharmaceutics
Pharmacokinetic and Pharmacodynamic Modelling in Drug Discovery and Development
Topic Editors: Inaki F. Troconiz, Victor Mangas Sanjuán, Maria Garcia-Cremades MiraDeadline: 31 August 2024

Conferences
Special Issues
Special Issue in
JPM
Novel and Personalized Treatment Concepts in Gynecologic Cancer
Guest Editors: Stephan Polterauer, Christoph GrimmDeadline: 30 April 2024
Special Issue in
JPM
Urogynecology: Insights in the Management, Treatment Approaches and Novel Therapies
Guest Editors: Themos Grigoriadis, Dimitrios Zacharakis, Anastasia ProdromidouDeadline: 20 May 2024
Special Issue in
JPM
Bioinformatics and Medicine
Guest Editors: Dorota Bielińska-Wąż, Piotr WążDeadline: 5 June 2024
Special Issue in
JPM
Pharmacogenomics from Research to Current Practice
Guest Editors: Xander Van Wijk, Natalie Reizine, Johannes MosbacherDeadline: 20 June 2024
Topical Collections
Topical Collection in
JPM
Genomic Medicine and Policy
Collection Editors: Christine Lu, Kurt Christensen, Nina Sperber
Topical Collection in
JPM
Advances of Emergency and Intensive Care
Collection Editor: Catalina Lionte